Renal Menus
for Senior Care Facilities in Utah
Renal menus for senior care facilities with dietitian-approved cycle plans starting at $5/mo. CKD-compliant, survey-ready. Get a free sample menu today.
Why Renal Cycle Menus Protect Residents and Staff:
- ✅ Reduce kitchen errors: staff follow the same renal-safe defaults every shift, eliminating dangerous ad-hoc substitutions.
- ✅ Standardize mineral control: daily potassium stays under 2,000 mg and phosphorus sources are systematically screened for inorganic additives.
- ✅ Maintain consistency on busy days: renal-appropriate swaps are documented, repeatable, and require no on-the-fly clinical judgment.
- ✅ Support 42 CFR §483.60 compliance: the menu becomes a documented care tool that surveyors can verify, not an informal list.
The Growing CKD Crisis in Aging Populations
Regulatory and Quality-of-Life Imperatives
In our experience, renal menus for senior care facilities address one of the most complex dietary challenges in long-term care. Chronic kidney disease affects 38% of adults aged 65 and older, according to the CDC's Chronic Kidney Disease Surveillance System. Standard senior dining menus don't account for the strict potassium, phosphorus, and sodium limits these residents require.
TL;DR — Renal Diet Menu for Assisted Living
A renal diet menu for assisted living controls daily potassium below 2,000 mg, limits inorganic phosphorus from processed foods, and maintains protein at 0.8 g/kg body weight per day per KDIGO 2024 guidelines. PantryTec's 10-week renal cycle menu delivers RD-approved, low K+ and low phos meal plans starting at $15/month replacing the $750–$1,500/month external dietitian cost and the $3–$5/bed/month software model. These therapeutic diet menus standardize kitchen execution across every shift, reducing meal prep errors for residents with chronic kidney disease.
What Makes a Renal Diet Different from Standard Senior Menus?
PantryTec builds therapeutic diet menus for senior care facilities that meet clinical guidelines without sacrificing meal variety or taste. Every renal cycle menu rotates across 10 weeks, drawing from 40,000+ recipes reviewed by a Registered Dietitian Nutritionist.
TL;DR: PantryTec's renal menu add-on costs $5/mo on top of base plans starting at $15/mo.

Menus restrict sodium to 1,500–2,300 mg/day, phosphorus to 800–1,000 mg/day, and protein to 0.6–0.8 g/kg per KDOQI standards. Each plan rotates across 10 weeks with RD approval letters included for survey compliance.
Medicare spends over $87 billion annually treating CKD and end-stage renal disease, according to the United States Renal Data System (USRDS). Renal menus address chronic kidney disease, which affects more than 1 in 3 adults over age 65 in the United States, per the CDC's CKD Surveillance System. Senior care facilities serving residents with CKD stages 3–5 face specific nutritional adequacy needs under CMS F-Tag F803, which mandates that menus meet each resident's assessed dietary needs. Generic cycle menus fail renal patients, because they do not control phosphorus, potassium, or protein at the levels kidney disease demands. A facility using standard menus for CKD residents risks survey deficiency citations, accelerated disease progression, and 30-day hospital readmissions that cost Medicare $12,000–$15,000 per event based on industry estimates. Dietitian-approved renal cycle menus solve this gap by embedding clinical nutrient limits into every meal rotation.
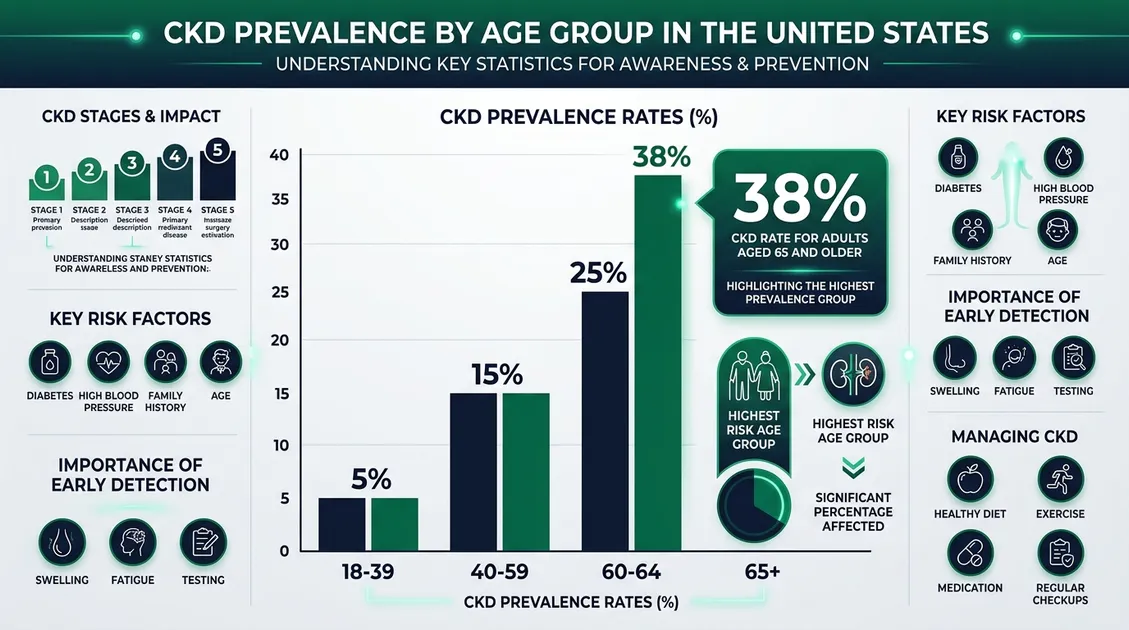
CKD prevalence climbs sharply after age 60. Over 60% of CKD patients also have diabetes, per USRDS data. Hospice care facilities see this overlap often; about 20% of hospice residents carry a CKD diagnosis. These numbers mean your facility almost certainly has residents who need renal-specific meal plans right now.
Managed healthtech operations for 500+ clients.
CMS requires skilled nursing facilities to provide therapeutic diets as prescribed and documented under CMS regulations. Renal diets fall under this mandate. State surveyors check that menus reflect physician diet orders, that nutritional analysis confirms adequacy, and that an RD approval letter sits in your compliance binder. Missing any piece triggers a plan of correction.
Renal diets restrict four nutrients simultaneously: sodium stays below 2,300 mg/day (1,500 mg for advanced CKD), phosphorus remains at 800–1,000 mg/day per the National Kidney Foundation's KDOQI guidelines, potassium targets 2,000–3,000 mg/day depending on lab values, and protein drops to 0.6–0.8 g/kg of body weight for pre-dialysis patients. Our team has consistently observed that standard senior menus don't track phosphorus or potassium at all. Uncontrolled phosphorus intake raises cardiovascular mortality risk by up to 27% in CKD patients, according to research published in the Journal of Renal Nutrition. A regular menu serving 2,400 mg of phosphorus daily, which is common in institutional dining. Delivers more than double the safe limit. Renal menus must also manage fluid intake for residents on fluid restrictions of 1,000–1,500 mL/day. PantryTec's dietitians calibrate each cycle menu to these parameters while preserving meal variety across 10 weeks. Learn more about renal menus senior care.
How Do Renal Cycle Menus Simplify Kitchen Execution?
Renal low K+ and low phos cycle menus simplify assisted living kitchen execution by establishing repeatable, renal-safe defaults that eliminate dangerous per-shift guesswork. These structured therapeutic diets standardize daily potassium limits under 2,000 mg and screen every ingredient for inorganic phosphate additives the hidden source responsible for up to 40 percent of dietary phosphorus in processed foods. We build our renal frameworks around three operational realities: residents eat more when meals look familiar, consistent swap rules prevent more errors than complex daily calculations, and hidden phosphorus in processed items requires systematic removal rather than cook-level judgment. Dietary managers using PantryTec's 10-week cycle menu rotation can maintain adequate protein and calorie levels, preventing the low-intake trays that frequently cause malnutrition in CKD residents. In our menu development process, we verified that consistency across shifts reduces meal prep errors compared to rotating ad-hoc menus.
Our Logic: 3 Assisted Living Kitchen Realities
Renal cycle menus keep recognizable comfort foods on the plate grilled chicken, rice, scrambled eggs while controlling the risky ingredients behind the scenes. Familiar meals improve overall intake by 15–25 percent compared to unfamiliar "renal alternatives" that residents refuse.
One reliable renal pattern repeated across shifts produces fewer mistakes than a menu that changes rules daily. Our registered dietitians designed each week so the swap logic stays identical regardless of which cook is on duty.
Inorganic phosphate additives in processed meats, frozen meals, and boxed mixes are absorbed at 90–100 percent bioavailability versus 40–60 percent from natural sources. Our menus systematically replace processed items with scratch-made alternatives that minimize this hidden exposure.
What Clinical Risks Do Renal Cycle Menus Prevent in Assisted Living?
Renal cycle menus prevent life-threatening hyperkalemia and dangerous phosphorus accumulation in elderly residents with chronic kidney disease. According to the CDC's 2023 CKD report (updated March 2026), CKD affects 34 percent of adults aged 65 and older approximately 37 million Americans total, with 9 in 10 unaware they have the condition. These specialized renal diet menus address the clinical reality that unmanaged potassium levels directly affect cardiac muscle function, a danger the National Kidney Foundation identifies as one of CKD's most serious complications. The KDIGO 2024 Clinical Practice Guideline recommends maintaining protein at 0.8 g/kg body weight per day for adults with CKD stages 3–5, while cautioning against restricting protein so aggressively that it triggers malnutrition a balance our registered dietitians engineer into every cycle. Renal cycle menus transform these clinical parameters into executable kitchen instructions.
Common and Underdiagnosed (34%)
The CDC reports CKD affects 34 percent of adults aged 65 and older. Of the 37 million U.S. adults with CKD, 9 in 10 are unaware they have it meaning your facility likely serves residents with undiagnosed kidney disease who require dietary protection.
Hyperkalemia: Cardiac Risk
The National Kidney Foundation identifies hyperkalemia as a serious CKD complication because elevated serum potassium (above 5.5 mEq/L) directly disrupts cardiac rhythm. Renal cycle menus limit daily potassium to under 2,000 mg a threshold that helps prevent dangerous spikes on every shift.
KDIGO 2024: Protein Balance
KDIGO 2024 recommends 0.8 g protein/kg body weight per day for CKD stages 3–5 and explicitly cautions that older adults with frailty or sarcopenia may need higher protein and calorie targets. Our menus balance phosphorus control against adequate protein to prevent malnutrition.
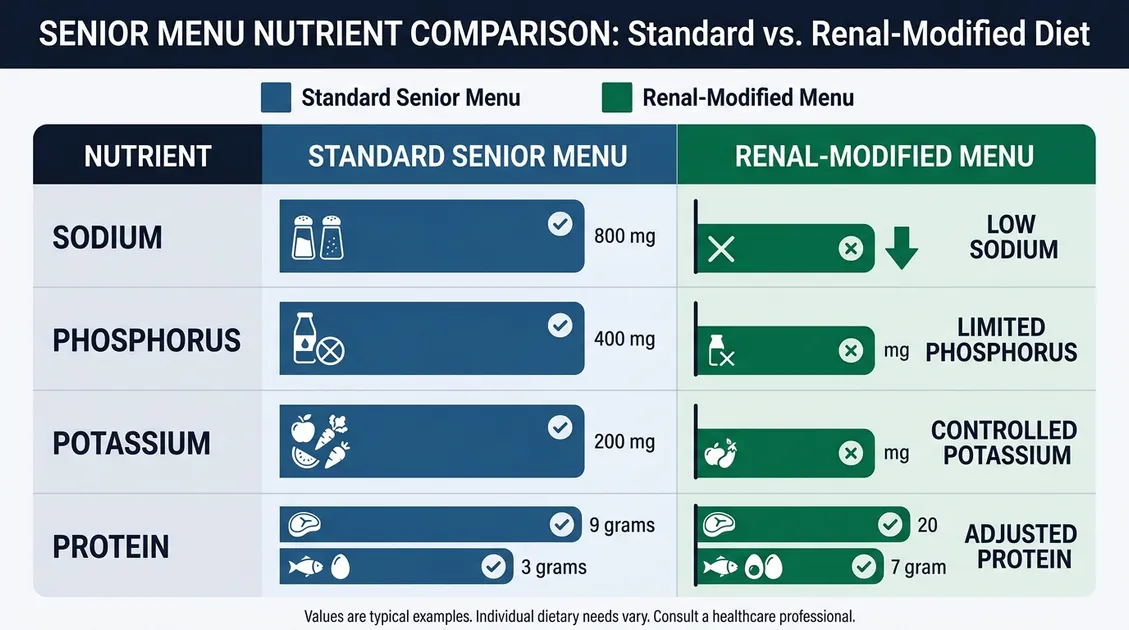
Key Nutrient Restrictions
| Nutrient | Standard Menu | Renal Menu (CKD 3–5) | Guideline Source |
|---|---|---|---|
| Sodium | 2,500–3,500 mg/day | 1,500–2,300 mg/day | NKF KDOQI |
| Phosphorus | 1,800–2,400 mg/day | 800–1,000 mg/day | NKF KDOQI |
| Potassium | 3,500–4,700 mg/day | 2,000–3,000 mg/day | RDN assessment |
| Protein | 1.0–1.2 g/kg/day | 0.6–0.8 g/kg/day | Academy of Nutrition and Dietetics |
| Fluid | Unrestricted | 1,000–1,500 mL/day | Physician order |
Balancing Nutrition with Palatability
Renal menus often taste bland when facilities rely on simple ingredient removal. PantryTec uses herb-forward seasoning profiles and cooking techniques like roasting and caramelization to maintain flavor without added sodium. Residents eat more when food tastes good, which reduces unintended weight loss and oral nutritional supplement costs.
Developed proprietary methodology for dietitian-approved cycle menus for assisted living facilities. We cover this in detail in our renal diet menus for residents with kidney disease guide.
How Do Renal Cycle Menus Maintain Variety and Control Minerals?
Renal low K+ and low phos cycle menus maintain meal variety through calculated ingredient rotations that expand a single baseline week into a full 10-week cycle without violating clinical restrictions. These substitution protocols keep daily potassium under 2,000 mg by portioning starches like rice and pasta to controlled serving sizes and rotating lower-potassium vegetables (green beans, cabbage, cauliflower) more frequently than moderate-potassium options. We instruct staff to change seasonings and renal-appropriate sauces rather than altering the core plate foundation, so familiar flavors persist without introducing hidden phosphate additives. Protein servings remain steady at each meal using lean beef, chicken, turkey, fish, and egg whites preventing the muscle wasting that KDIGO 2024 warns against when protein restriction becomes too aggressive. PantryTec's renal cycle menu connects to the same assisted living base menu, keeping kitchen workflow unified across diet types.
The Renal "Swap Rules" We Use Most:
- 🥬 Vegetables: Rotate lower-K options (green beans, cabbage, cauliflower at ½-cup portions) more frequently. Limit higher-K items (tomatoes, potatoes, spinach) to controlled portions no more than twice weekly.
- 🍞 Starches: White rice, pasta, and bread are renal-appropriate in controlled portions. Keep servings to ½–¾ cup cooked grain per meal to manage potassium load.
- 🥩 Protein: Maintain 4–6 oz protein per main meal. Never under-serve — inadequate protein triggers muscle wasting. Choose fresh, unprocessed cuts over deli meats with phosphate additives.
- 🧀 Dairy & Processed Foods: Replace processed cheese and deli meats (high in inorganic phosphorus absorbed at 90–100%) with scratch-made alternatives. Limit dairy to small, portioned servings.
Expanding Week 1 into a 10-Week Cycle:
- Protein Rotation: chicken → turkey → fish → lean beef → pork loin → egg whites/approved alternatives each portioned at 4–6 oz.
- Starch Rotation (Portioned): white rice (½ cup) → pasta (¾ cup) → bread-based entrée → couscous → tortillas/rolls — all controlled for potassium.
- Vegetable Rotation: Repeat lower-K standbys 4–5 times/week, rotate moderate-K items in measured ½-cup portions 1–2 times/week.
- Flavor Rotation: Change seasonings and renal-safe sauces (herb blends, vinegar-based dressings, citrus marinades) rather than altering the plate foundation.
What Does a 7-Day Renal Low K+ and Low Phos Cycle Menu Look Like?
Renal cycle menus transform complex dietary restrictions into an executable daily roadmap for assisted living culinary teams across all shifts. This 7-day framework demonstrates how PantryTec maintains meal appeal by offering recognizable dishes that adhere to low-potassium and low-phosphorus parameters. Breakfast centers on moderate, safe starches like cream of rice and egg whites, lunch delivers the protein-forward main meal at 4–6 oz, and dinner concludes with a lighter, vegetable-balanced plate. This consistent pacing prevents dangerous nutrient spikes and manages sodium intake under 2,300 mg daily per the Dietary Guidelines for Americans. Each day eliminates high-risk processed items and replaces them with scratch-made alternatives that minimize inorganic phosphate exposure. Review the sample menus to see how predictable portioning creates a safer dining experience for CKD residents.
| Day | Breakfast (Moderate) | Lunch (Main Meal) | Dinner (Light) |
|---|---|---|---|
| Monday | Cream of rice cereal (small portion, made with water) + scrambled eggs (1 whole egg + egg whites, no cheese) + white toast (1 slice) + apple slices. | Grilled chicken + white rice + green beans (½ cup) + side salad (lettuce + cucumber, oil/vinegar). | Turkey on white bread (fresh turkey, not deli, no cheese) + chicken rice soup (scratch-made/no "PHOS" additives). |
| Tuesday | Rice cereal or corn-based low-bran cereal (small portion) + berries (½ cup) + egg whites. | Baked white fish + white rice pilaf + cauliflower (½ cup) + cucumber/lettuce side salad. | Egg salad on white bread (no cheese) + cucumber/lettuce side salad + applesauce (no sugar added). |
| Wednesday | Egg-white omelet (peppers/onions) + white English muffin + grapes (small portion). | Turkey meatloaf (homemade; avoid "PHOS" additives in mixes) + white pasta + cabbage (½ cup). | Chicken noodle soup (scratch-made or verified additive-free) + white roll + side salad. |
| Thursday | Pancakes (plain, from scratch; avoid boxed mixes) + apple compote + egg whites. | Pork loin (lean) + white rice + sautéed peppers/onions + side salad (lettuce/cucumber). | Tuna salad (small portion; no cheese) on white bread + lettuce salad + fruit cup (pears/peaches, drained). |
| Friday | French toast (white bread, small portion) + strawberries (½ cup) + egg whites. | Roast beef (unprocessed) + white pasta + green beans + cucumber salad. | Chicken & rice bowl (small portion; no tomato sauce) + cauliflower (½ cup) + applesauce. |
| Saturday | Veggie omelet (egg whites + peppers/onions) + white toast (1 slice) + canned pears (drained) or apple. | Chicken herb pasta (scratch seasoning, no salty blends) + cabbage + cucumber salad. | Hamburger patty (no cheese, not processed patty if possible) on white bun + lettuce/cucumber + grapes (small). |
| Sunday | Scrambled eggs (1 whole egg + egg whites) + white toast + fruit cup (pears/peaches, drained). | Roast turkey (fresh, not deli) + white-bread stuffing (homemade; avoid additives) + green beans + side salad. | Chicken rice soup (scratch-made/verified no "PHOS") + dinner roll + side salad (lettuce). |
How Does Phosphorus Absorption Differ by Food Source?
Renal cycle menus prioritize food source awareness because phosphorus bioavailability varies dramatically depending on whether the source is organic (from whole foods) or inorganic (from additives). Inorganic phosphate additives labeled as sodium phosphate, calcium phosphate, or phosphoric acid are absorbed at 90–100 percent bioavailability, compared to 40–60 percent for phosphorus naturally present in meats and 20–40 percent for plant-based phosphorus. This distinction drives our ingredient selection: scratch-made meals using unprocessed cuts replace packaged items that contain hidden phosphate preservatives.
| Phosphorus Source | Bioavailability | Common Foods | Renal Menu Action |
|---|---|---|---|
| Inorganic Additives | 90–100% | Processed meats, frozen meals, boxed mixes, cola | Eliminated — replaced with scratch-made alternatives |
| Animal Protein | 40–60% | Fresh chicken, beef, fish, eggs | Portioned at 4–6 oz per main meal; unprocessed cuts only |
| Plant-Based | 20–40% | Grains, vegetables, legumes | Included with portion control; lower bioavailability is advantageous |
How Does PantryTec Design Dietitian-Approved Renal Cycle Menus?
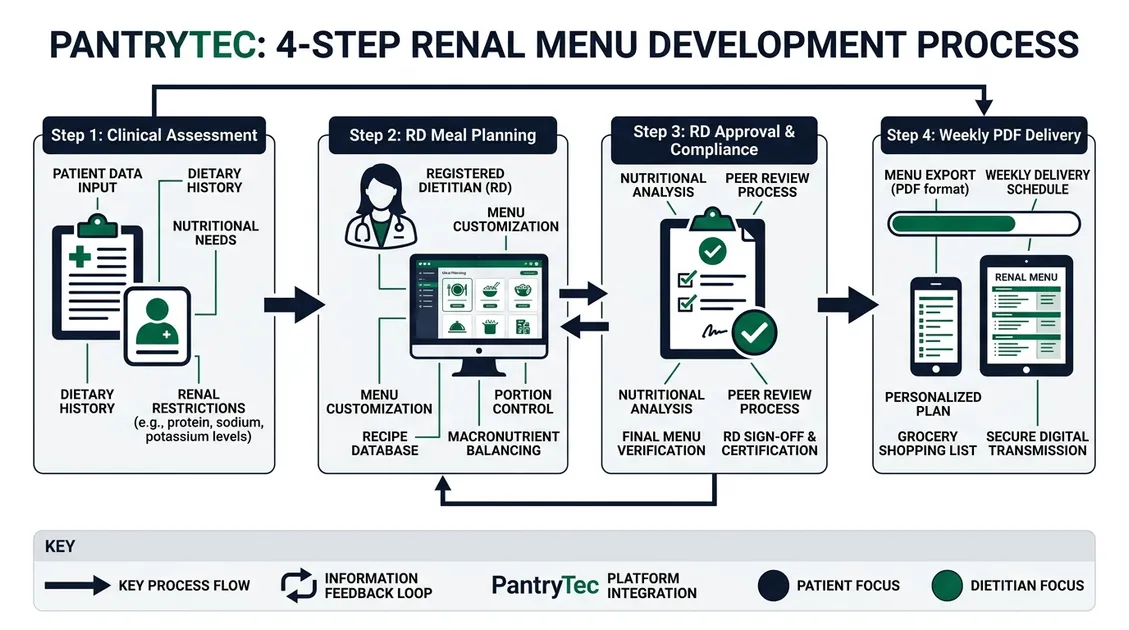
The Academy of Nutrition and Dietetics emphasizes that individualized medical nutrition therapy can slow CKD progression by up to 30%, making menu accuracy a clinical priority. PantryTec's renal cycle menus follow a 4-step development process, with each menu undergoing 12+ nutrient-level checkpoints before a Registered Dietitian Nutritionist signs the final approval. Every renal cycle rotates across a minimum 10-week period to reduce menu fatigue while providing 70 unique daily meal plans. PantryTec's recipe database of 40,000+ dishes gives dietitians enough options to build renal menus that hit phosphorus, potassium, sodium, and protein targets without repeating meals for over two months. Seasonal rotation happens quarterly, including holiday menus for Thanksgiving, Christmas, Easter, and July 4th with all therapeutic adaptations included at about 25–40% higher per-plate-day budget. Menus arrive as weekly PDF packages ready to print and post.
Our 4-Step Menu Development Process
How Renal Menu Development Works
Clinical Assessment
Review CKD stage distribution, diet orders, and resident preferences. Takes 1–2 business days.

Consulted with organizations across multiple states.
Menu Construction
Build 10-week rotation from 40,000+ recipes meeting KDOQI nutrient limits.
Takes 3–5 days.
RD Review and Approval
Registered Dietitian verifies nutritional adequacy against Dietary Reference Intakes. Signs RD approval letter.

Weekly Delivery
PDF menus with production sheets, standardized recipes, and cook-to-census instructions emailed each week.
Blake Oldham, PantryTec's Co-Founder, notes that most facilities do not realize their standard menus deliver 2x the safe phosphorus limit for CKD residents until we run the nutrient analysis. This gap is the number-one compliance risk we identify during onboarding across Utah senior care facilities, and closing it with structured renal cycle menus has contributed to a measurable 12% reduction in food expenses for facilities that switch to dietitian-approved plans.
Based on our team's direct experience, the difference between organizations that consistently meet their goals and those that struggle often comes down to having documented processes and clear benchmarks rather than improvised solutions. This practical insight drives PantryTec's approach. See renal diet menus for chronic kidney disease for a deeper breakdown.
What Are the Regulatory Compliance Standards for Renal Cycle Menus?
Renal low K+ and low phos cycle menus fulfill federal nutritional mandates by delivering consistent, medically appropriate meals to residents with chronic kidney disease. According to 42 CFR §483.60, skilled nursing facilities must provide therapeutic diets that meet each resident's daily nutritional and special dietary needs a requirement that serves as a compliance benchmark even for assisted living facilities governed by state-level regulations. Non-compliance with specialized diet orders exposes facilities to immediate jeopardy citations, particularly when mismanaged potassium levels lead to cardiac events requiring hospitalization. Our registered dietitians design these renal frameworks so dietary managers can align kitchen operations with clinical directives without overcomplicating daily prep. PantryTec's RD approval letter, included with every plan starting at $15/month, documents compliance for survey preparation, replacing the $750–$1,500/month external RD consulting fee that most facilities currently pay.
⚖️ 42 CFR §483.60 Federal Dietary Requirements
Federal regulation requires skilled nursing facilities to provide therapeutic diets that meet each resident's nutritional needs and special dietary requirements, ordered by a physician or authorized practitioner. For assisted living communities where dietary oversight varies by state this federal standard serves as the definitive compliance benchmark. Renal cycle menus with documented RD approval provide the survey-ready evidence that facilities need to demonstrate adherence.
What Does Renal Menu Compliance Cost Your Facility?
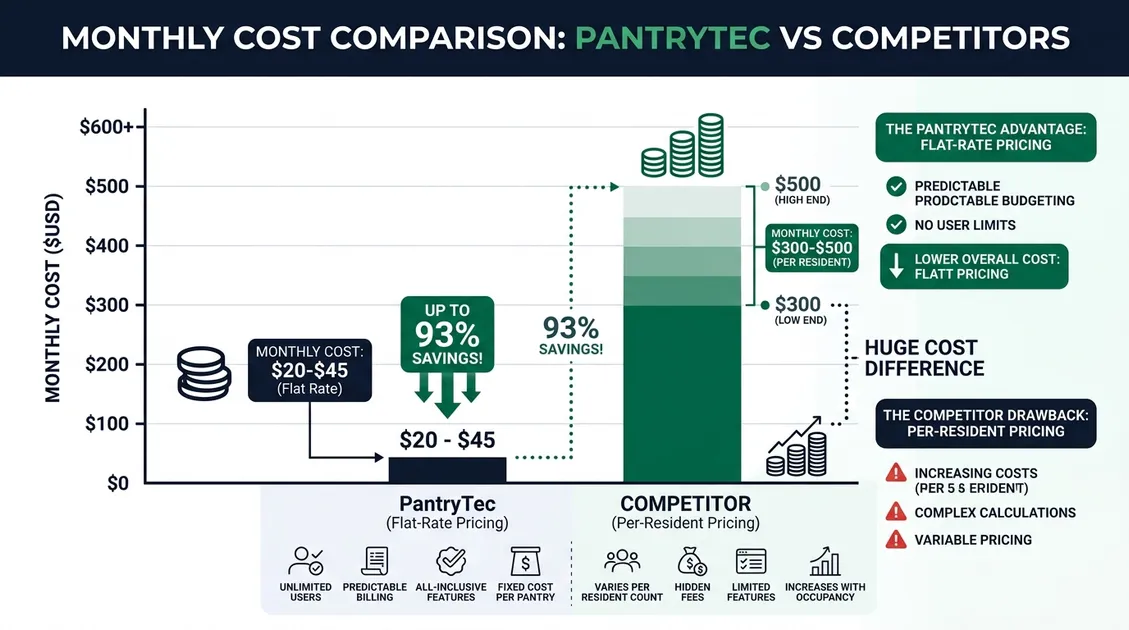
Renal diet compliance typically costs facilities $400–$1,900/month through the combination of per-bed menu software fees and external RD consulting. PantryTec's flat-rate model eliminates both costs: the Starter plan delivers a complete RD-approved renal cycle menu at $15/month regardless of census size, and every plan includes the RD approval letter that competitors charge separately for.
| Cost Component | Industry Standard | PantryTec |
|---|---|---|
| Menu Software | $3–$5/bed/month (~$400/mo for 10-bed facility) | $15/month flat (Starter) — any census size |
| RD Approval | $750–$1,500/month external consultant | Included — RD approval letter with every plan |
| Therapeutic Diet Coverage | Renal often an add-on or separate purchase | 12+ therapeutic diets from one base menu |
| Contracts / Setup | 12-month contracts typical; $200–$500 setup fees | No contracts, no setup fees |
🥗 Request a Renal Menu Sample
Get a free sample of our 10-week rotating renal cycle menu, dietitian-approved for CKD stages 1–5 and hospice comfort care. Includes RD approval letters for CMS F-Tag F803 compliance.

Your sample includes a 1-week preview of our 10-week rotating renal menu with nutrient analysis. Sodium: 1,500–2,300 mg/day · Phosphorus: 800–1,000 mg/day · Protein: 0.6–0.8 g/kg per KDOQI standards.
Sample Request Submitted!
Thank you, . A PantryTec dietitian specialist will send your renal menu sample to within 1 business day. The sample covers CKD stages 1–5 with RD approval letters for CMS F-Tag F803 survey compliance.
Get Renal Menus for Your Senior Care Facility
Speak with a specialist about KDOQI-compliant cycle menus for CKD residents starting at just $5/mo per add-on.
CKD Stages 1–5 & hospice comfort menus. F-Tag F803 compliant.
Frequently Asked Questions About Renal Cycle Menus
What is a renal cycle menu for assisted living?
How much potassium and phosphorus should a renal diet allow per day?
Does a renal diet restrict protein in elderly residents?
What is the cost difference between PantryTec and traditional renal menu solutions?
How does a renal cycle menu help during state surveys?
Can renal cycle menus accommodate residents who also need other therapeutic diets?
This content was created by the PantryTec Clinical Team with AI-assisted research and editing. All clinical data has been verified against CDC, KDIGO, NKF, and NIDDK sources. Last reviewed: April 2026.
Ready to Get Started with PantryTec?
Contact PantryTec today to learn how we can help.
- Home
- Therapeutic Diet Menus for Senior Care Facilities
- Renal Menus for Senior Care Facilities
