Low Sodium Senior Menus
for Therapeutic Diets
Low sodium senior menus with ≤1,500 mg sodium per day, dietitian-approved for assisted living. PantryTec plans start at $15/mo. Get a free sample menu.
How Excess Sodium Impacts Senior Health Outcomes
TL;DR: Low sodium senior menus restrict daily intake to ≤1,500 mg sodium while boosting potassium to 3,500–4,200 mg. PantryTec delivers these menus as weekly print-ready PDFs starting at $15/mo. With RD approval letters included.
What Is the Sodium-Potassium Balance and Why Does It Matter?
In our experience, therapeutic add-ons cost $5/mo. No contracts, no software to learn.
Low sodium menus for seniors are the most often prescribed therapeutic diet menus in senior care facilities, driven by the fact that nearly 80% of adults aged 65 and older have hypertension. PantryTec builds dietitian-approved low sodium senior menus for assisted living, memory care, and skilled nursing communities across Utah. Each menu caps sodium at 1,500 mg per day while pairing potassium-rich ingredients to support cardiovascular health. Plans start at $15 per month, a 96% cost reduction compared to facilities paying $400 or more elsewhere for the same compliance documentation.

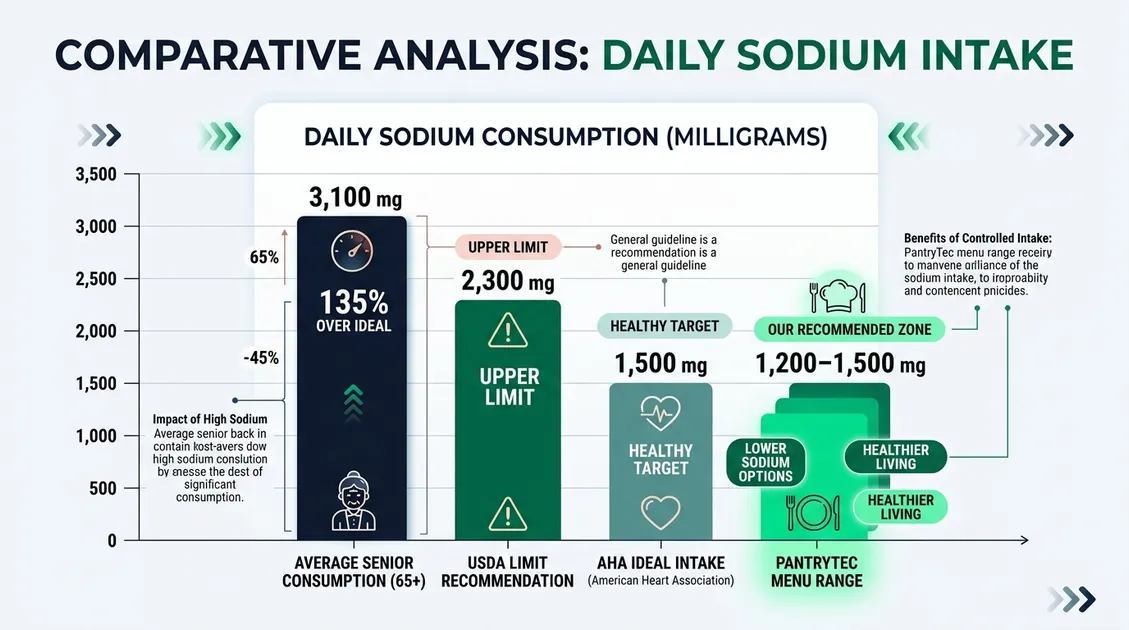
Low sodium therapeutic diets reduce systolic blood pressure by 5–6 mmHg in older adults, according to AHA clinical data. Low sodium senior menus address a measurable health crisis: Americans aged 65 and older consume an average of 3,100 mg of sodium per day, more than double the 1,500 mg recommended by the American Heart Association. Senior care facilities face regulatory obligations under CMS F-Tag F803 to serve meals meeting each resident's nutritional needs, and sodium management ranks among the most scrutinized areas during state surveys. PantryTec's low sodium cycle menus hold each entrée to ≤600 mg sodium, with full-day totals between 1,200 mg and 1,500 mg. The 2020–2025 USDA Dietary Guidelines for Americans set an upper limit of 2,300 mg for the general population, though the AHA's ideal target for adults with hypertension remains 1,500 mg. Facilities without structured low sodium menus risk dietary deficiency citations during inspections, which account for roughly 12% of all skilled nursing survey findings, based on CMS CASPER data.
Excess sodium intake accelerates fluid retention, elevates blood pressure, and increases stroke risk among aging adults. Seniors metabolize sodium less efficiently due to declining kidney function. A resident consuming 3,100 mg daily faces 2× the cardiovascular event risk compared to one eating ≤1,500 mg, per AHA longitudinal studies. Low sodium senior menus built by a Registered Dietitian Nutritionist account for these physiological changes in every meal.

Managed healthtech operations for 500+ clients.
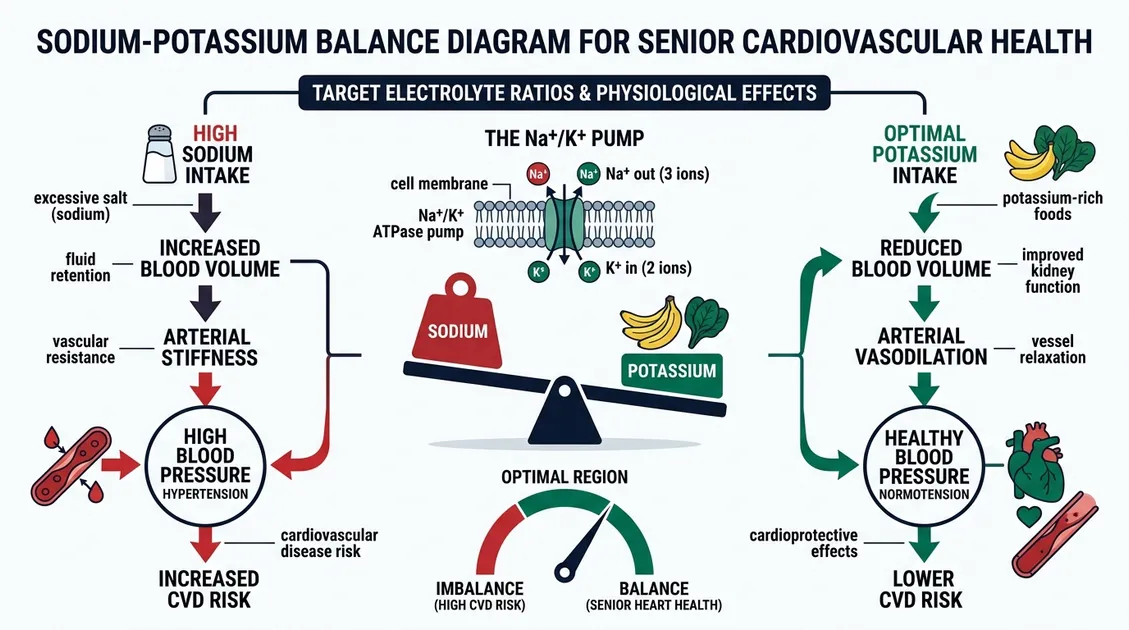
Sodium-potassium balance refers to the dietary ratio between these two electrolytes, and a ratio below 1:1 (sodium-to-potassium) is associated with a 20% lower risk of cardiovascular mortality, according to the World Health Organization. PantryTec's low sodium senior menus target 1,200–1,500 mg sodium paired with 3,500–4,200 mg potassium per day, maintaining a ratio well below 1:1. Only 2% of Americans meet the adequate potassium intake of 4,700 mg per day, making deliberate menu engineering essential for senior care. Potassium-rich foods like sweet potatoes, white beans, bananas, and spinach appear in every PantryTec cycle rotation. Each recipe undergoes nutrient analysis tracking 28 or more micronutrients to verify the sodium-potassium ratio holds across breakfast, lunch, dinner, and snacks. This dual-focus approach doesn't just reduce sodium, it actively strengthens the electrolyte balance that protects cardiac function in residents aged 65 and older.
Dietitian-Approved Cycle Menus for Senior Care Facilities hear from Utah assisted living administrators that their biggest concern about low sodium diets is resident acceptance. Kitchen managers worry meals will taste bland. PantryTec addresses this by layering citrus acids, fresh herbs, and umami-rich ingredients like tomato paste and mushrooms into every recipe flavor strategies that maintain satisfaction scores while keeping sodium under therapeutic thresholds.
Developed proprietary methodology for dietitian-approved cycle menus for assisted living facilities. Learn more about low sodium menus seniors.
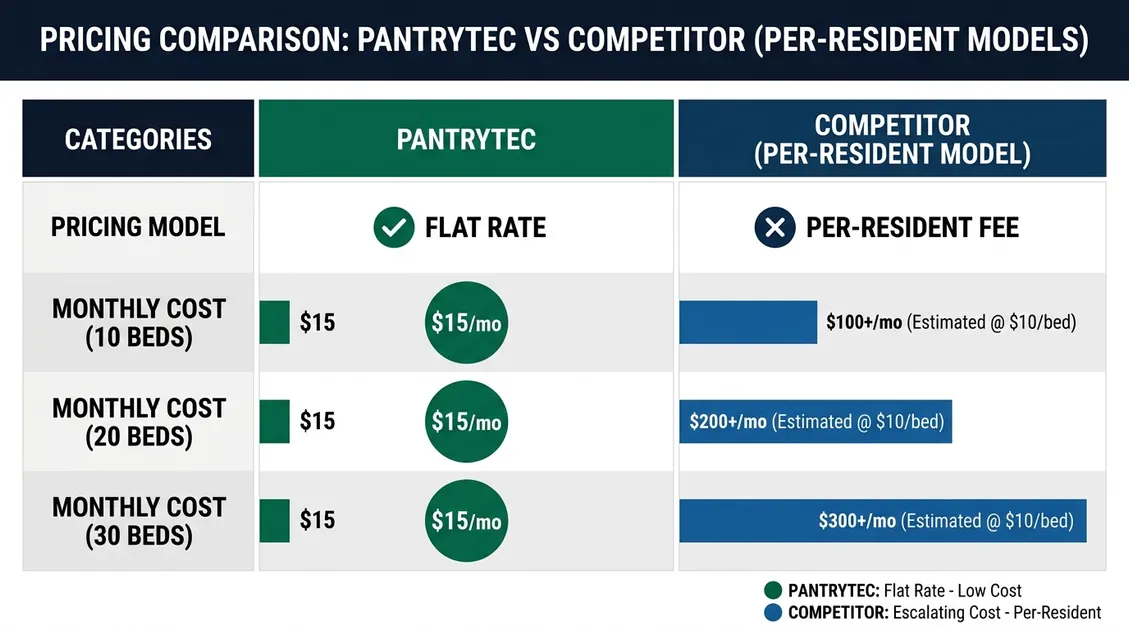
💰 Per-Resident Cost Savings Calculator
See how much your facility can save switching to PantryTec's low sodium menus starting at just $15/mo with RD approval included.
📊 Cost Breakdown Comparison
* PantryTec plans start at $15/mo with RD approval included. Therapeutic low sodium add-on is $5/mo. No contracts required. Savings calculated by comparing your current dietitian consulting spend against PantryTec's all-inclusive pricing. Food cost PPD used for per-resident context.
How Do PantryTec's Dietitian-Approved Cycle Menus Reduce Sodium?
The Academy of Nutrition and Dietetics recommends cycle menus of at least 3–4 weeks for nutritional variety in long-term care. PantryTec's low sodium cycle menus use a 10-week rotating framework with 70 unique daily meal plans before any repetition, drawn from a database of over 40,000 recipes reviewed for therapeutic compliance. Each entrée stays at or below 600 mg sodium. Full daily totals hold between 1,200 mg and 1,500 mg. PantryTec exceeds that standard with a 10-week rotation that delivers 700 or more unique meals across a full cycle. A Registered Dietitian Nutritionist reviews every menu before deployment. The RD Approval Letter ships with each cycle, ready for your compliance binder at zero additional cost. PantryTec offers three menu styles: Homemade Focus, Premade Focus, and Weekend Hybrid. Facilities switch between styles at any time without contract penalties. Weekly PDF delivery includes production sheets, standardized recipes with portion control instructions, and cook-to-census guidelines scaled to your resident headcount.
Flavor Without the Salt: Culinary Techniques in Every Rotation
Low sodium senior menus from PantryTec replace table salt with herb blends, acid brightness from lemon and vinegar, and natural umami from roasted tomatoes. Garlic, onion powder, cumin, and smoked paprika add depth. These techniques maintain resident satisfaction without exceeding the 600 mg-per-entrée cap. Standardized recipes ensure every dietary aide replicates the same flavor profile regardless of staff turnover.

Consulted with organizations across multiple states.
| Therapeutic Diet | Daily Sodium Target | Daily Potassium Target | Key Restriction |
|---|---|---|---|
| General Low Sodium | ≤1,500 mg | 3,500–4,200 mg | No added salt, low-sodium ingredients |
| AHA Cardiac Diet | ≤1,500 mg | 3,500–4,700 mg | Sodium + saturated fat + cholesterol limits |
| Renal Diet (CKD Stage 3–4) | ≤2,000 mg | Monitored per lab values | Sodium + potassium + phosphorus controlled |
| Diabetic / Consistent Carb | ≤2,300 mg | Standard RDA | Carbohydrate consistency per meal |
| Heart Failure (CHF) | ≤1,500 mg | Per physician order | Sodium + fluid restriction |
Based on our team's direct experience, the difference between organizations that consistently meet their goals and those that struggle often comes down to having documented processes and clear benchmarks rather than improvised solutions. This practical insight drives PantryTec's approach. We cover this in detail in our low sodium menus for senior residents guide.
What Therapeutic Diet Conditions Require Low Sodium Menus?
About 37% of adults with CKD also have hypertension, requiring dual-focus sodium and potassium management. Low sodium therapeutic diet menus serve residents with hypertension, congestive heart failure, chronic kidney disease, and diabetes-comorbid cardiovascular conditions. Congestive heart failure affects about 6.7 million Americans aged 20 and older, per the American Heart Association, with sodium restriction as a dietary management priority. The National Kidney Foundation states CKD patients should consume no more than 2,000 mg of sodium per day, with potassium monitored based on disease stage. PantryTec's AHA cardiac low sodium menu plans go beyond general sodium reduction by adding saturated fat and cholesterol limits. Renal diet menus for chronic kidney disease layer phosphorus restrictions on top of sodium caps. Managing overlapping conditions from a single base menu is where most facilities struggle and where PantryTec's 40,000-recipe database proves its value.

Blake Oldham, PantryTec's Co-Founder, notes that facilities managing 3 or more therapeutic diet types from a single kitchen always report the highest compliance stress. A scenario our team encounters regularly involves a new resident admission requiring simultaneous low sodium, renal, and diabetic changes. PantryTec's menu system generates each therapeutic extension automatically from the base cycle, so kitchen staff print one document per diet type zero manual recipe calculation required. See renal diet menus for chronic kidney disease for a deeper breakdown.
Get RD-Approved Low Sodium Menus for Your Facility
Speak with PantryTec about dietitian-approved cycle menus capping sodium at ≤1,500 mg/day plans starting at just $15/mo with RD approval letters included.
No obligation. Ask about F-Tag F803 compliance & 96% cost savings.
💡 On desktop? Dial (385) 512-4731 from your phone.
2 Gm Sodium Restriction Menus
For Assisted Living Facilities.
2 gm sodium menus transform cardiovascular care in senior living facilities. A 2 gm sodium restriction strictly limits total dietary sodium intake to exactly 2,000 mg per day to manage fluid retention and heart health.
Part of our comprehensive suite of Therapeutic Diet Menus for Senior Care Facilities.
Why Do 2 Gm Sodium Menus Matter for Assisted Living Facilities?
2 gm sodium menus restrict total daily dietary sodium intake to a maximum of 2,000 milligrams to manage chronic cardiovascular conditions and prevent fluid retention in elderly residents. A 2-gram sodium diet means limiting sodium strictly to 2,000 mg daily, which is significantly lower than the general U.S. Dietary Guidelines advising 2,300 mg per day. These specialized cycle menus reduce both clinical risks for residents and operational risks for dining staff by providing clear, standardized guardrails against high-sodium ingredients. According to the World Health Organization, keeping adult sodium intake under 2,000 mg daily serves as a critical global benchmark for heart health. Standardized 2 gm sodium menus prevent survey deficiencies by ensuring facilities meet complex nutritional and special dietary needs reliably across every shift. Understanding the specific differences between "low salt" preparation and strict 2,000 mg caps helps clinical teams confidently manage resident health.
Regulatory Compliance
Federal regulation 42 CFR § 483.60 mandates that the facility must provide each resident a nourishing diet that meets daily nutritional and special dietary needs, considering preferences. This specifically encompasses F-tag 808 compliance for therapeutic diets.
The 2,000 mg Threshold
A 2 gm sodium restriction enforces a daily cap of 2,000 mg. The U.S. Dietary Guidelines advise general daily limits of 2,300 mg for adults, meaning therapeutic cardiac diets operate on a much tighter restriction to combat edema and hypertension.
FDA "Low Sodium" Definition
"Low sodium" labeled products contain exactly 140 mg or less per serving. Dietary managers must verify this FDA nutrient content claim guidance before allowing packaged items onto the cycle menu.
How Do Facilities Execute 2 Gm Sodium Menus Effectively?
2 gm sodium menus require strict process control in the kitchen, specifically mandating no added salt during cooking or table service, alongside the use of verified low-sodium products. Facilities execute these therapeutic diets by minimizing processed foods, which typically conceal the majority of dietary sodium. Dietary managers must exclusively source items labeled "low sodium," meaning the product contains exactly 140 mg of sodium or less per serving according to current FDA nutrient content claim guidance. 2 gm sodium menus eliminate high-risk deli meats, replacing them with fresh turkey to keep the daily sodium budget realistic and predictable. Kitchen staff rely on acid-based flavor enhancers like fresh lemon juice, herbs, and vinegar to create highly palatable plates without compromising the strict 2,000 mg daily limit. Mastering these practical culinary adjustments ensures successful compliance while preserving the dignity and satisfaction of assisted living residents during mealtime.
No Added Salt
2 gm sodium menus forbid salt added in cooking or at the table. Cooks must use salt-free seasoning blends.
Zero Deli Meats
Processed meats hide extreme sodium levels. Use fresh roasted turkey and chicken exclusively.
Verify Broths & Breads
Scratch-made soups or verified low-sodium broths (≤140 mg per serving) are mandatory for compliance.
What Does a 1-Week 2 Gm Sodium Menu Look Like?
2 gm sodium menus structure daily meals to maintain total intake safely near the 2,000 mg limit while offering familiar, comforting regular texture foods that residents enjoy. This one-week menu cycle covers exactly 7 full days of meals, demonstrating how carefully selected ingredients create balanced, flavorful plates without relying on heavy salt additions or processed shortcuts. 2 gm sodium menus feature scratch-made elements like unsalted butter eggs, fresh roasted chicken, and carefully verified low-sodium broth soups to strictly control the nutritional baseline. Dining directors must verify that every bread roll and soup base aligns with the 140 mg per serving FDA definition to prevent accidental sodium spikes. Our comprehensive menus standardize these safe products, allowing cooks to execute repeatable, compliant meals efficiently even during busy shifts or unexpected staffing shortages. Reviewing this structured cycle provides a clear blueprint for maintaining steady flavor profiles within cardiovascular dietary restrictions.
| Day | Breakfast (Moderate) | Lunch (Main Meal) | Dinner (Light) |
|---|---|---|---|
| Monday | Eggs (no salt) cooked with unsalted butter + low-sodium toast + melon | Chicken (lemon/herb, no skin) + plain potato (no salt) + green beans | Fresh turkey (not deli) + low-sodium broth soup (turkey/veg) |
| Tuesday | Oatmeal (water) + cinnamon + berries + egg whites | Lemon-herb chicken + plain potato + carrots | Fresh turkey sandwich on "no added sodium" bread (no cheese/mayo) + low-sodium broth soup |
| Wednesday | Scrambled eggs (no salt) + low-sodium toast + peaches (fresh or no-salt cup) | Baked white fish + plain rice + zucchini | Turkey and noodle soup (low-sodium broth) + soft dinner roll (low sodium) + side salad (oil/vinegar) |
| Thursday | Cream of wheat (water) + fruit + egg whites | Chicken (herb) + plain potato + cauliflower | Fresh turkey plate (gravy-free) + low-sodium broth soup + steamed veg |
| Friday | Pancakes (from scratch, no added salt) + fruit topping + eggs (no salt) | Chicken (lemon/herb) + plain pasta + green beans | Turkey and rice soup (low-sodium broth) + soft cooked carrots |
| Saturday | French toast (no added salt) + berries + egg whites | Chicken (herb) + plain potato + mixed vegetables | Fresh turkey on low-sodium toast + low-sodium broth soup |
| Sunday | Eggs (no salt) with unsalted butter + low-sodium toast + melon | Roast chicken (no skin, herb) + plain potato + green beans | Fresh turkey + low-sodium broth soup + side salad (oil/vinegar, no-salt dressing) |
What Are the Key RD Approval Rules for 2 Gm Sodium Menus?
2 gm sodium menus must pass rigorous registered dietitian review by explicitly restricting daily total sodium intake to approximately 2,000 mg and eliminating all high-sodium deli meats. As of 2026, clinical compliance requires dining teams to strictly verify that any included packaged foods, especially broths and breads, meet the strict 140 mg per serving low-sodium threshold. 2 gm sodium menus often intersect with other clinical needs, requiring thoughtful adjustments for residents managing complex fluid restrictions or those who require specialized texture modifications. We design PantryTec's cycle menus to support appetite and hydration naturally, offering warm broth-based soups and no-salt-added fruit options that align with strict cardiovascular protocols. Standardizing one approved salt-free seasoning blend and one reliable soup base prevents the silent sodium accumulation that frequently causes cycle menus to fail regulatory audits. Implementing these defined approval rules guarantees consistent, survey-ready nutritional care across all facility operations.
Nursing Home Execution Notes
- • Chewing-Friendly: Keep meats moist using lemon and herb juices. Avoid excessively crunchy sides for residents with oropharyngeal difficulties.
- • Appetite Support: Combat flavor fatigue by offering no-salt-added applesauce or fresh fruit.
- • Standardize Safety: Ensure CNAs and cooks use exactly one approved salt-free seasoning blend to eliminate guesswork.
Common Staff Questions
Not always. "No added salt" describes the cooking process. A 2 gm sodium restriction is a firm mathematical daily limit. Unchecked broths can ruin a no-added-salt meal.
Sometimes, but it must be precisely measured. To keep execution foolproof, this Week 1 menu excludes them entirely.
Read more FAQs, learn who this diet is for, or view a sample preview.
Ready to Get Started with PantryTec?
Contact PantryTec today to learn how we can help.
- Home
- Therapeutic Diet Menus for Senior Care Facilities
- Low Sodium Senior Menus
