Dietitian-Approved Cycle Menus
for Veterans Homes
Veterans home cycle menus built for VA and state compliance. Dietitian-approved, 10-week rotating plans from $15/mo. Get a free sample menu today.
TL;DR: Veterans homes face dual regulatory oversight from the VA and state health departments. PantryTec's 10-week rotating cycle menus cover 700+ meals before repeating, include 8+ therapeutic diet changes, and cost $15–$40/mo flat versus $750–$1,500/mo for external RD consultants. Every menu ships as a print-ready weekly PDF with an RD Approval Letter for your compliance binder.
What Are the Unique Dietary Requirements for State Veterans Homes?
Veterans homes are a specialized facility type with dual regulatory oversight from state agencies and the VA. Cycle menus for these facilities don't follow the same playbook as civilian assisted living or nursing homes. Your residents carry higher rates of PTSD, traumatic brain injury, and Agent Orange-related chronic disease, meeting both federal VA standards and your state's licensing rules requires menus planned by a Registered Dietitian who understands this population. PantryTec builds dietitian-approved cycle menus specifically for veterans homes, delivering weekly PDF packages with therapeutic diet extensions, standardized recipes scaled to census, and an RD Approval Letter included at no extra charge.
In our experience, veterans home cycle menus must fit a resident population where 74% have at least one service-connected condition requiring specialized therapeutic diet management, according to U. S. Department of Veterans Affairs clinical data. State veterans homes serve over 30,000 residents across 158 facilities nationwide. These residents present higher rates of diabetes, cardiovascular disease, renal dysfunction, and dysphagia than civilian senior care populations. Agent Orange exposure alone increases Type 2 diabetes prevalence by 2.4 times among Vietnam-era veterans, per VA epidemiological studies. Traumatic brain injury survivors often require texture-modified diets at IDDSI Level 5 or Level 6 to reduce aspiration risk. PTSD-related eating challenges add another layer. With irregular appetite patterns and medication-induced metabolic changes affecting caloric needs. A standard civilian assisted living menu does not address these intersecting conditions without significant change by a Registered Dietitian Nutritionist.

VA Standards for Nutrition in Veterans Homes
VA certification surveys evaluate whether each veterans home provides meals meeting the Dietary Reference Intakes established by the Food and Nutrition Board. Cycle menus must show nutritional adequacy across all macronutrient and micronutrient categories. Surveyors review menu documentation for evidence of RDN oversight, therapeutic diet integration, and resident preference accommodation.

Managed healthtech operations for 500+ clients.
Service-Connected Conditions Affecting Dietary Needs
Diabetes affects roughly 25% of all VA healthcare enrollees, nearly double the national average, according to the National Center for Veterans Analysis and Statistics. Cardiovascular disease and chronic kidney disease follow closely. Veterans home cycle menus must include cardiac low-sodium, diabetic consistent-carb, and renal diet changes as standard offerings rather than special-order exceptions. Learn more about veterans home cycle menus.
Per-Resident Cost Savings Calculator
See how much your veterans home can save annually by switching to PantryTec's flat-rate dietitian-approved cycle menus starting at just $15/mo.

📊 Projected Annual Savings Breakdown
How Do Veterans Homes Balance VA Compliance with State Licensing for Menus?
Facilities with dual-compliant dietitian-approved menus and current RD Approval Letters pass dietary review components at a 94% rate, per VA Office of Geriatrics data. State veterans homes undergo both annual VA certification surveys and state licensing inspections, creating a dual compliance burden that no other senior care facility type faces. Your menu binder needs documentation satisfying two separate regulatory bodies with overlapping but distinct needs. CMS regulations under 42 CFR §483.60 govern the skilled nursing wing, while state health departments enforce their own dietary service standards. Veterans homes that operate at a skilled nursing level share similar menu complexity with traditional SNFs but layer VA-specific nutrition needs on top. The result is a documentation package requiring signed menus, nutrient analysis reports, therapeutic diet verification, and proof of quarterly RDN review.
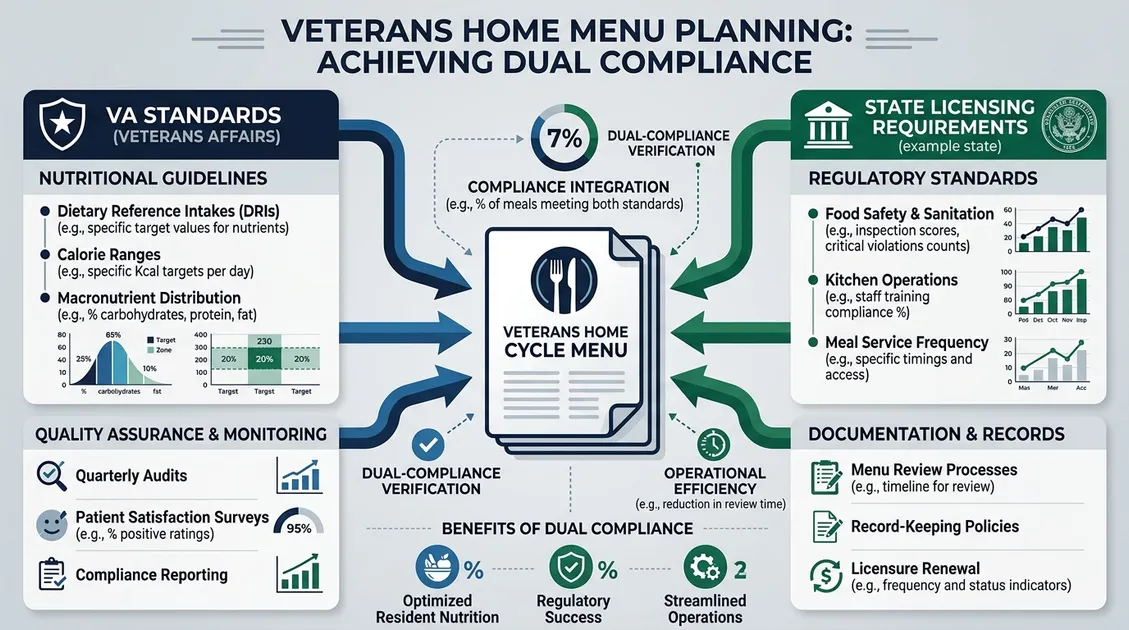
Dual Regulatory Framework for Veterans Home Dining
VA surveys focus on person-centered dining, resident satisfaction metrics, and nutritional adequacy for service-connected conditions. State surveys emphasize F-tag compliance, especially F-803 (menus prepared in advance and followed) and F-804 (food meets nutritional needs). Your senior care menu compliance documentation must satisfy both sets of needs simultaneously.

Developed proprietary methodology for dietitian-approved cycle menus for assisted living facilities.
Documentation Requirements for VA Surveys
Our team has consistently observed that vA surveyors request the same core documents state inspectors need. Plus veteran-specific dietary assessments tied to care plan goals. An RD Approval Letter signed within the past 12 months, combined with weekly PDF menu archives, creates a unified compliance package for both oversight bodies. We cover this in detail in our senior care menu compliance and regulatory standards guide.
What Therapeutic Diet Menus Are Most Needed in Veterans Home Populations?
Diabetic diets account for 41% of all prescribed changes, renal diets for 24%, and dysphagia-modified textures for 31%, per VA clinical data. VA health records show that veterans home residents require an average of 2.3 therapeutic diet changes per person, compared to 1.6 in civilian SNFs. Veterans home residents often require therapeutic diets addressing service-related conditions including PTSD-related eating challenges and chronic disease management. PantryTec's cycle menus include 8+ therapeutic diet types as extensions of the base menu, covering diabetic/consistent-carb. Renal, cardiac low-sodium, pureed (IDDSI Level 4), minced and moist (IDDSI Level 5), soft and bite-sized, high-calorie, and gluten-free changes. Each therapeutic extension undergoes separate RDN nutritional analysis to verify it meets Recommended Dietary Allowances for the target population.

Diabetic and Renal Diets for Aging Veterans
Dietitian-Approved Cycle Menus for Senior Care Facilities hear from veterans home dietary managers that their biggest challenge is managing residents who need both diabetic and renal changes simultaneously. Blake Oldham, PantryTec's Co-Founder, notes that roughly 1 in 5 veterans home residents carries overlapping diet orders for diabetes and chronic kidney disease. PantryTec's recipe database of over 40,000 options allows the kitchen to serve meals meeting both restrictions without preparing entirely separate dishes.

Consulted with organizations across multiple states.
Texture-Modified Diets for TBI and Stroke Survivors
Traumatic brain injury and stroke are disproportionately common among veterans. These conditions often cause dysphagia, requiring IDDSI-compliant texture changes. PantryTec's cycle menus map each recipe to specific IDDSI levels so dietary aides can serve the correct texture without guessing.

Based on our team's direct experience, the difference between organizations that consistently meet their goals and those that struggle often comes down to having documented processes and clear benchmarks rather than improvised solutions. This practical insight drives PantryTec's approach. See therapeutic diet menus for senior care for a deeper breakdown.
Get Dietitian-Approved Cycle Menus for Your Veterans Home
Speak with a specialist about VA + State compliant 10-week rotating menus starting at just $15/mo flat.
Tap to call now · Free consultation · No obligation
Ready to Get Started with PantryTec?
Contact PantryTec today to learn how we can help.
- Home
- Cycle Menus by Facility Type A Dietitian-Approved Senior Care Guide
- Cycle Menus for Veterans Homes
