AHA Cardiac Low Sodium/Fat Cycle
Menu.
A Cardiac Low Sodium Menu provides essential cardiovascular and hepatic support for residents across senior care facilities. Reliable nutrition that protects vulnerable patients without requiring complex culinary overhauls.

Part of our complete suite of Therapeutic Diet Menus for Senior Care Facilities.
Why Does a Cardiac Low Sodium Menu Matter for Facility Compliance?
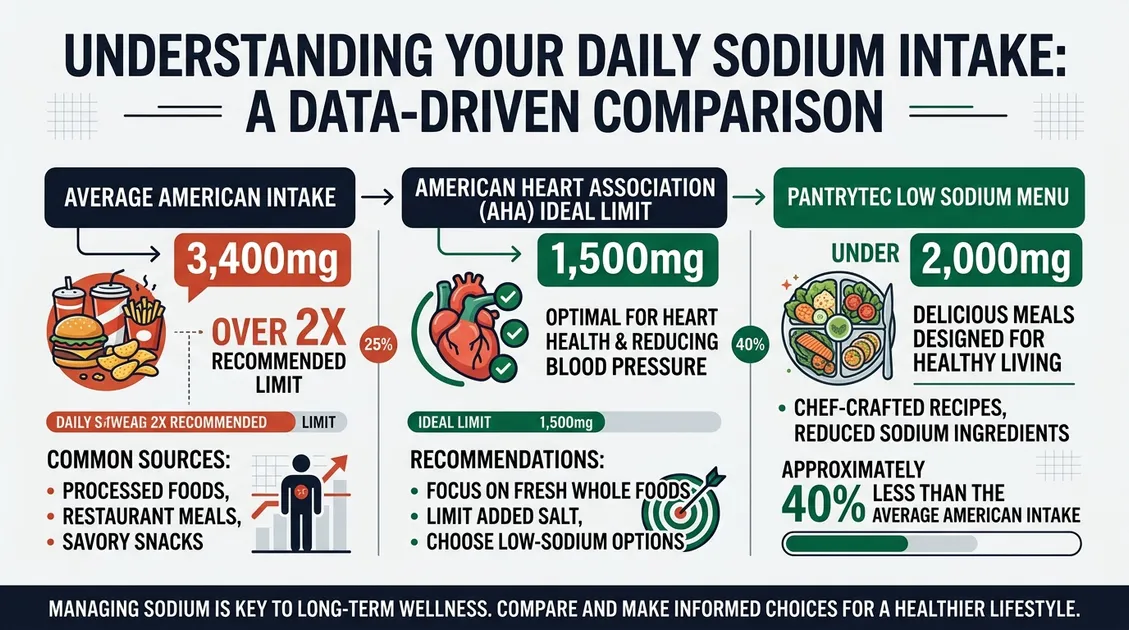
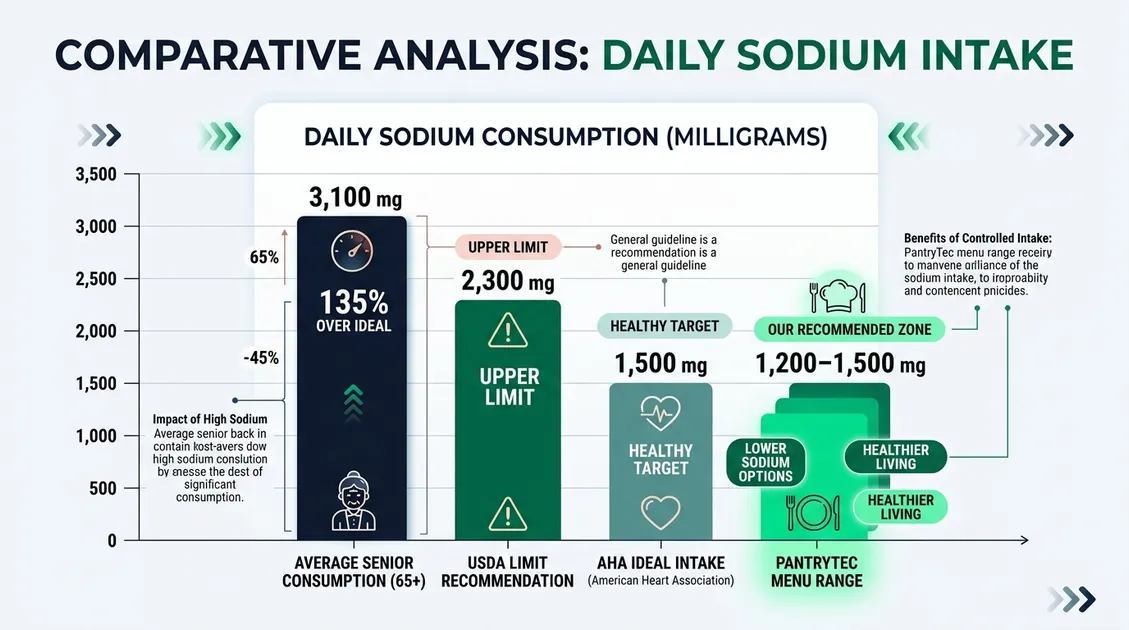
Low sodium and low fat menus establish a repeatable clinical standard that prevents life-threatening cardiovascular events while ensuring regulatory alignment during nursing home surveys. PantryTec's cycle menus target American Heart Association guidelines, restricting daily sodium intake to a maximum of 2,300 milligrams and optimally remaining below 1,500 milligrams per day for vulnerable adult populations. Low sodium and low fat menus standardize kitchen execution, directly reducing accidental high-fat plate errors by utilizing precise starch anchors and standardized protein portions across all dietary shifts. Under federal regulation 42 CFR § 483.60, dietary managers face strict scrutiny during 2026 state surveys if therapeutic diets deviate from physician orders or fail to meet documented nutritional requirements. Low sodium and low fat menus eliminate guesswork by relying on scratch-made, no-salt bases and fresh, unbrined proteins rather than high-sodium convenience foods. Facilities adopting this structured approach consistently demonstrate better survey readiness while providing residents with dignified, appetizing meal options that protect against hidden sodium spikes.
AHA Clinical Daily Targets (2,000 kcal Reference Diet)

| Nutrient | AHA Upper Limit | Optimal Target | Clinical Rationale |
|---|---|---|---|
| Sodium | 2,300 mg/day | < 1,500 mg/day | Reduces hypertension risk |
| Total Fat | 35% of calories | 25–30% of calories | Supports hepatic function |
| Saturated Fat | < 6% of calories | < 13.3 g/day | Lowers LDL cholesterol |
| Trans Fat | 0 g (avoid entirely) | 0 g | Directly elevates cardiac risk |
| Added Sugars | < 10% of calories | < 25 g/day (women), < 36 g/day (men) | Reduces metabolic burden |
| Fiber | N/A (minimum target) | 25–30 g/day | Supports lipid clearance |
F-Tag Readiness
Documenting sodium assumptions keeps the menu survey-ready. If a soup is scratch-made, the standardized recipe must legally specify "no added salt." When facilities utilize commercial products, they must maintain a verified low-sodium list tracking brand names, exact sodium content per serving, storage locations, and pre-approved substitutes to seamlessly pass registered dietitian (RD) reviews.
What Defines a Cardiac Low Sodium Menu Clinically?
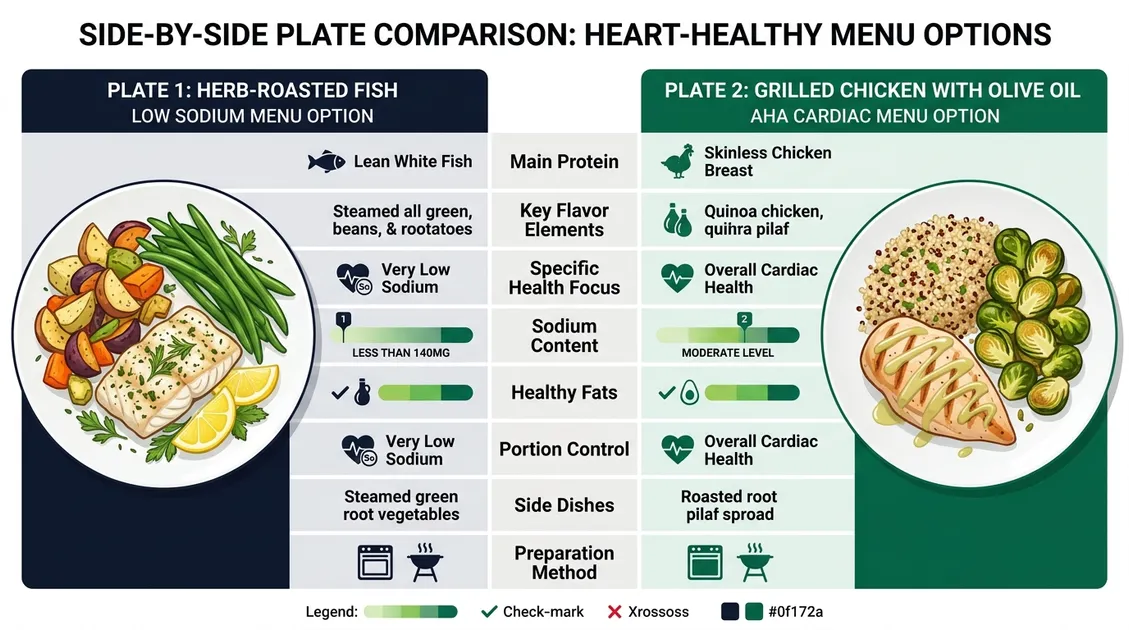

Low sodium and low fat menus restrict total daily fat intake to a maximum of 35 percent of calories while maintaining saturated fat below 6 percent. Low sodium and low fat menus demand rigorous ingredient sourcing, ensuring a 2,000-calorie daily diet contains fewer than 13.3 grams of saturated fat. PantryTec's cycle menus achieve precise macronutrient targets by replacing heavy cream sauces with lean proteins like egg whites, skinless chicken breast, and fresh turkey. Low sodium and low fat menus utilize dry-heat cooking methods including baking, grilling, and roasting to preserve flavor without introducing unnecessary lipids. Research underscores the danger of hidden sodium within processed deli meats and canned soups, which rapidly push a patient past the 2,300-milligram daily ceiling. Low sodium and low fat menus build flavor using acidic elements like lemon juice, garlic, and salt-free herbal blends instead of relying on butter. This framework ensures residents enjoy palatable meals supporting optimal gallbladder and hepatic function.
Lean Protein Sourcing
Therapeutic efficacy requires fresh, unbrined proteins. Deli turkey and pre-seasoned meats carry massive sodium loads that instantly violate cardiac guidelines.
Dry-Heat Cooking
Kitchens must standardize their preparation methods. Baking, steaming, grilling, and roasting ensure the meals remain easily digestible for gallbladder patients.
Strategic Flavoring
Flavor without fat is an operational system. We build taste using aromatic onions, lemon, vinegar, and salt-free seasoning blends instead of salty broths.
Sodium-Smart Ingredient Swap Reference
Kitchen teams eliminate hidden sodium by replacing high-load ingredients with therapeutically equivalent alternatives.
| Avoid (High Sodium) | Sodium Load | Swap For | Sodium Saved |
|---|---|---|---|
| Deli turkey (2 oz) | ~720 mg | Fresh roasted turkey breast | ~650 mg |
| Canned soup base (1 cup) | ~890 mg | Scratch stock + salt-free herbs | ~820 mg |
| Table salt (¼ tsp) | ~580 mg | Lemon juice + garlic + herbs | ~580 mg |
| Soy sauce (1 tbsp) | ~900 mg | Low-sodium tamari (1 tsp) | ~700 mg |
| Mayonnaise (2 tbsp) | ~190 mg + 22 g fat | Low-fat Greek yogurt + dill | ~150 mg + 20 g fat |
| Cheddar cheese (1 oz) | ~180 mg + 6 g sat fat | Olive oil + red wine vinegar | ~180 mg + 6 g sat fat |
| Bouillon cube (1) | ~1,150 mg | No-sodium vegetable base | ~1,100 mg |
| Butter (1 tbsp) | ~90 mg + 7 g sat fat | Olive oil spray / infused oil | ~90 mg + 6 g sat fat |
How Do Low Sodium and Low Fat Menus Prevent Hidden Fat Creep?
Low sodium and low fat menus require strict operational guardrails to prevent quiet fat accumulation from untracked butter additions, creamy salad dressings, and unmeasured starch portions. Low sodium and low fat menus treat bread slices, rice scoops, and pasta servings as strict caloric anchors that must remain identical across every patient tray. PantryTec's cycle menus implement precise measurement protocols utilizing standardized scoops and ladles to eliminate free-pouring habits that inflate daily saturated fat totals. Low sodium and low fat menus swap traditional mayonnaise for low-fat Greek yogurt and replace rich cheese garnishes with olive oil and vinegar combinations. CNAs and dietary teams frequently compromise cardiac diets through small additions during plate finishing, making continuous staff training critical for maintaining nutritional fidelity across changing kitchen shifts. Low sodium and low fat menus prioritize consistency over perfection, establishing a reliable daily rhythm that guarantees therapeutic efficacy. Implementing these defensive cooking strategies empowers senior care operators to confidently serve heart-healthy meals without relying on constant managerial oversight.
The Starch Anchor Problem
Diet breakdowns frequently occur when starch portions drift. Extra rolls or free-poured pasta quietly change the entire macronutrient profile of a resident's meal without the kitchen noticing.
Eliminating Fat Creepers
Defaults protect the diet. We train staff to recognize "fat creepers" like butter on toast or oily sauté steps. Swapping mayonnaise for yogurt-based spreads saves hundreds of calories.
Daily Macronutrient Distribution (2,000 kcal Cardiac Plan)
| Macronutrient | % of Calories | Daily Grams | Primary Sources |
|---|---|---|---|
| Carbohydrates | 50–55% | 250–275 g | Whole grains, fruits, vegetables |
| Protein (Lean) | 15–20% | 75–100 g | Skinless poultry, fish, egg whites |
| Total Fat | 25–30% | 55–65 g | Olive oil, avocado, nuts |
| — Saturated Fat | < 6% | < 13.3 g | Minimal dairy, no butter |
| Fiber | — | 25–30 g | Oats, beans, vegetables |
| Sodium | — | < 1,500–2,300 mg | Natural food sodium only |
F-Tag Compliance Quick Reference for Cardiac Diets
Dietary managers must document every therapeutic assumption behind a cardiac menu to pass state surveys under 42 CFR § 483.60. Use the table below as a pre-survey audit checklist covering the four F-tags most frequently cited for low sodium and low fat menu violations in long-term care.
| F-Tag | Regulatory Focus | Cardiac Menu Requirement | Documentation Proof |
|---|---|---|---|
| F-692 | Nutrition & Hydration Status | Resident receives calorie-adequate cardiac meals | Weekly nutrition intake logs |
| F-693 | Tube Feeding Mgmt. | N/A unless resident on enteral support | Physician order + RD review |
| F-803 | Menus & Nutritional Adequacy | Approved cycle menu meets AHA targets & RDA | RD-signed nutrient analysis |
| F-804 | Nutritive Value / Appearance / Taste | Low-sodium meals remain palatable & appetizing | Resident satisfaction surveys |
| F-805 | Food in Form to Meet Needs | Texture-modified cardiac meals when ordered | IDDSI level documentation |
| F-806 | Resident Food Preferences | Substitutes honored within cardiac parameters | Signed preference interview form |
| F-812 | Food Safety Requirements | Scratch stocks & proteins stored correctly | Temperature logs + HACCP records |
One-Week AHA Cardiac Low Sodium and Low Fat Cycle Menu
Low sodium and low fat menus deliver structured, seven-day meal rotations designed specifically for long-term care kitchens balancing cardiovascular health with practical daily execution. Low sodium and low fat menus eliminate the unpredictability of daily meal planning by providing kitchen staff with a verified, medically appropriate template for breakfast, lunch, and dinner services. Our cycle menus prioritize fresh, unprocessed ingredients, incorporating baked cod, turkey meatloaf, and vegetable-forward pasta primavera to maintain daily sodium totals between 80 milligrams and 420 milligrams per primary meal. Low sodium and low fat menus require culinary teams to prepare soups from scratch without added salt, avoiding the catastrophic sodium inflation commonly associated with commercial soup bases. Facilities implementing these specific cycles can seamlessly integrate new culinary staff, as the therapeutic logic remains constant even when the specific protein or vegetable rotation shifts during subsequent weeks. Low sodium and low fat menus ultimately bridge the gap between rigorous medical requirements and the practical realities of high-volume nursing home foodservice operations.
| Day | Breakfast (Moderate) | Lunch (Main Meal) | Dinner (Light) |
|---|---|---|---|
| Monday | Eggs (no salt) + toast (low-sodium bread) + melon ~200-300 mg Na |
Chicken (no skin) + mashed potatoes (no salt) + green beans ~80-160 mg Na |
Fresh turkey (no deli) on toast + low-sodium soup ~280-420 mg Na |
| Tuesday | Oatmeal (water) + cinnamon + berries + egg whites ~150-240 mg Na |
Baked white fish + herb rice + steamed carrots ~110-190 mg Na |
Chicken & veg soup (low sodium) + side salad ~160-260 mg Na |
| Wednesday | Egg-white veggie omelet + toast + fruit cup ~240-340 mg Na |
Turkey meatloaf (lean) + pasta (plain/herb) + cabbage ~110-200 mg Na |
Tuna salad (low-sodium) on toast + cucumber ~180-300 mg Na |
| Thursday | Plain low-fat Greek yogurt + sliced peaches + toast ~130-220 mg Na |
Pork loin (lean) + no-salt mash + green beans ~70-150 mg Na |
Low-sodium veg soup + half chicken salad sandwich ~270-410 mg Na |
| Friday | French toast (no added salt) + strawberries ~120-220 mg Na |
Roast turkey (fresh) + rice pilaf + mixed vegetables ~170-300 mg Na |
Baked cod + cauliflower + side salad ~90-170 mg Na |
| Saturday | Scrambled eggs (no salt) + toast + melon ~200-300 mg Na |
Chicken breast + pasta primavera (veg-forward) ~160-260 mg Na |
Turkey & rice soup (low sodium) + steamed zucchini ~150-240 mg Na |
| Sunday | Pancakes (plain, no added salt) + fruit topping ~170-280 mg Na |
Roast beef (lean) + mashed potatoes + green beans ~60-140 mg Na |
Veg & barley soup (low sodium) + dinner roll ~250-380 mg Na |
Who Should Receive Low Sodium and Low Fat Menus in Senior Care?

Low sodium and low fat menus specifically support residents managing gallbladder dysfunction, fat intolerance symptoms, and physician-ordered cardiovascular interventions requiring strict dietary modifications. Low sodium and low fat menus provide critical nutritional stabilization for patients exhibiting discomfort after consuming rich, heavily processed food items typical in standard facility dining. Our therapeutic regimens explicitly target cardiac-style needs, intentionally avoiding the fried foods and heavy cheese dishes that contribute to escalating lipid panels and hypertension among elderly populations. Low sodium and low fat menus must not be utilized for residents requiring high-calorie interventions for unplanned weight loss, nor are they appropriate for individuals managing complex renal restrictions involving phosphorus or potassium limits without explicit clinical adjustments. Dietary managers must secure formal approval from a registered dietitian before assigning this specific meal plan to patients requiring precise diabetic carbohydrate controls or specific dysphagia texture modifications. Low sodium and low fat menus serve as a foundational clinical tool, ensuring the right patient receives the optimal nutritional intervention.
Dietary Contradictions (RD Review Required)
- ⚠️ Weight Loss: Not suitable for residents facing unplanned weight loss who require calorie-dense interventions.
- ⚠️ Renal Limits: Do not use if the resident has strict potassium, phosphorus, or fluid restrictions.
- ⚠️ Strict Sodium Caps: While low sodium, patients with severe restrictions below 1,500mg require highly customized, verified product sourcing.
Protect Residents. Ensure Survey Readiness.
Get AHA-compliant cardiac cycle menus delivered directly to your kitchen for just $15/month.
- Home
- Therapeutic Diet Menus for Senior Care Facilities
- AHA Cardiac Low Sodium Menu
