Dietitian Approved Menus
for Assisted Living Facilities
Dietitian-approved cycle menus for assisted living start at $15/mo flat-rate. RD approval letters included.
TL;DR: Over 30 states require dietitian involvement in assisted living menus. PantryTec delivers 10-week rotating cycle menus with RD approval letters starting at $15/mo — replacing $750–$1,500/mo external dietitian costs. Plans cover 8+ therapeutic diets, 40,000+ recipes, cook-to-census instructions, and wholesale price comparison across Sysco. US Foods, and Walmart.
Why Do Assisted Living Communities Need Dietitian-Approved Menus?
Assisted living cycle menus for senior care facilities must meet nutritional adequacy standards set by both state licensing agencies and CMS §483.60 regulations. A Registered Dietitian Nutritionist reviews each menu for calorie targets, macronutrient balance, micronutrient thresholds, and therapeutic diet compliance before signing a formal approval letter.PantryTec's dietitian-approved cycle menus handle this entire process for your facility at a flat monthly rate, no per-resident fees, no contracts, no software to learn. You receive print-ready PDF menus each week, complete with standardized recipes, shopping lists scaled to census, and a signed RD approval letter for your survey binder.
Watch: How Dietitian-Approved Cycle Menus Work in Assisted Living

See how PantryTec delivers weekly menus, RD approval letters, and shopping lists to your facility with zero software training required.
In our experience, dietitian-approved menus are required in over 30 states for assisted living communities, according to the National Center for Assisted Living's 2024 regulatory review, with non-compliant facilities facing fines of $1,500–$10,000 per citation. Assisted living residents transfer from nursing homes at increasing rates, yet their nutritional needs remain medically complex. The California HealthCare Foundation's report on home care for the elderly found that at most 10 to 20 percent of nursing home residents with only physical or cognitive impairments qualify as candidates for assisted living transfer. Those who do transition carry dietary needs for therapeutic changes, micronutrient monitoring, and texture adjustments that demand professional oversight. PantryTec builds each cycle menu to meet Dietary Reference Intakes for calories (1,800–2,200 kcal/day for seniors). Protein (60–80 g/day), sodium (under 2,300 mg/day), and potassium (2,600–3,400 mg/day for adults 51+). Your facility receives a signed RD approval letter proving compliance.

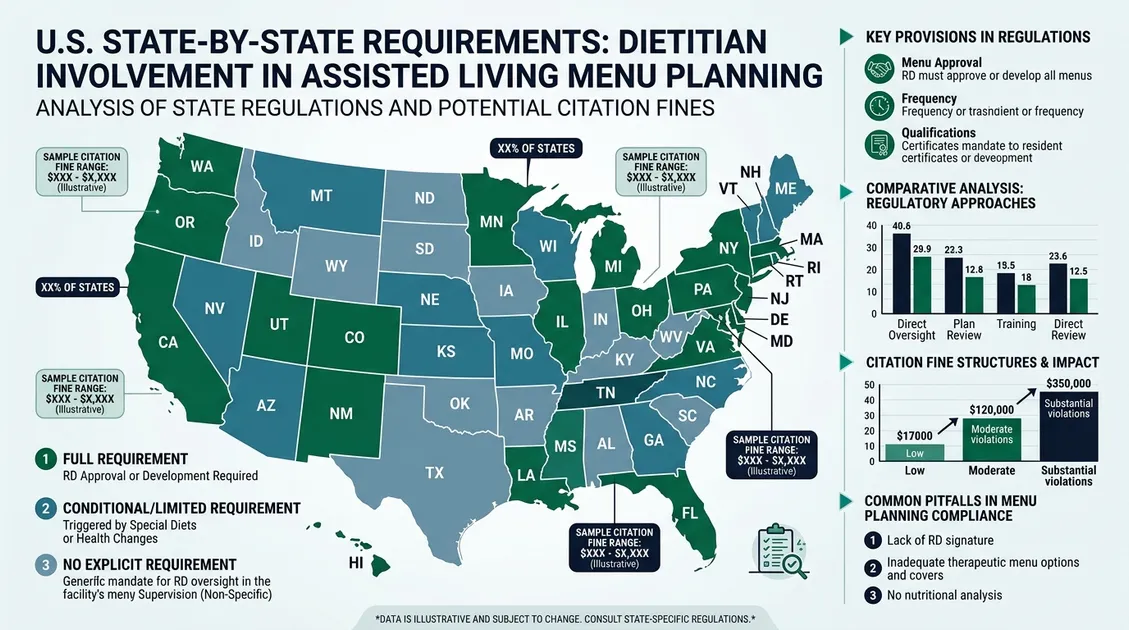
State-by-State Assisted Living Menu Regulations
Assisted living dietary regulations vary sharply across states. Utah's Bureau of Health Facility Licensing requires meals approved by a licensed dietitian under R432-270. California's Title 22 §87555 mandates RCFE facilities maintain dietitian-reviewed menus on file.
Some states accept a national RD's remote signature, while others require a locally licensed practitioner. CMS F-Tag F803 specifies that menus meet each resident's nutritional needs, and F-Tag F804 requires qualified dietitian involvement in the planning process.
Managed healthtech operations for 500+ clients.
How Assisted Living Dietary Needs Differ From Skilled Nursing
Assisted living residents have greater meal autonomy than skilled nursing populations. Liberalized diet policies allow more food choices, selective menus, and restaurant-style dining. Skilled nursing facilities follow stricter CMS meal pattern mandates and 14-hour meal spacing rules under F-Tag F809.

Understanding menu differences across facility types ensures your meal planning matches the correct regulatory framework. Assisted living menus balance resident choice with nutritional adequacy, a narrower regulatory lane, but one that still requires documented RDN oversight. Learn more about assisted living cycle menus.
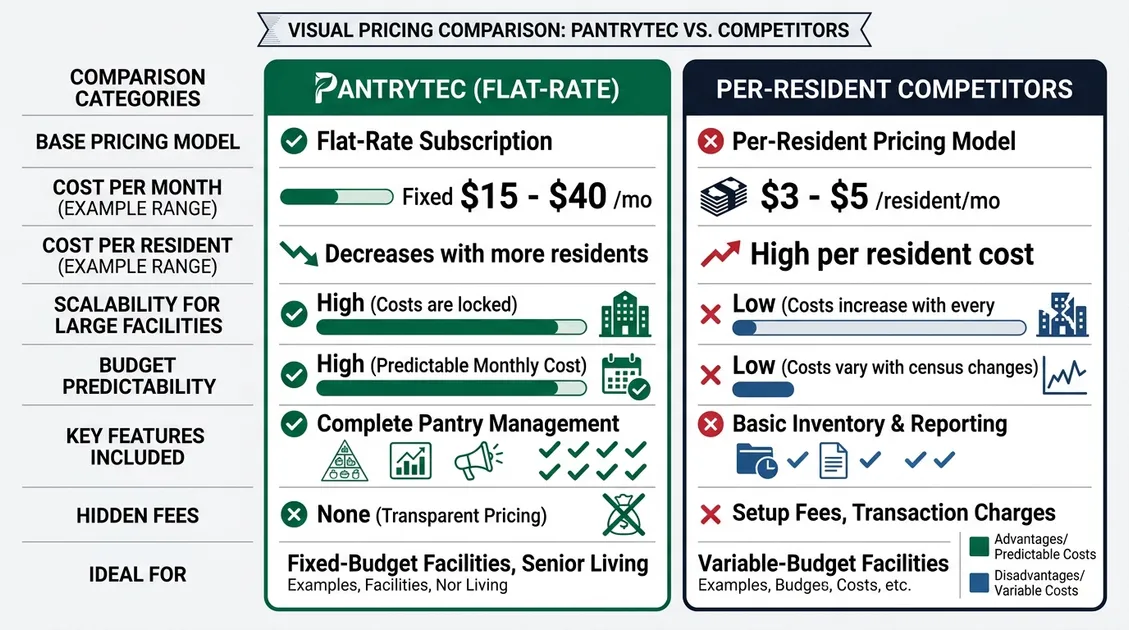
💰 Per-Resident Cost Savings Calculator PantryTec
See how much your facility can save annually with PantryTec's flat-rate dietitian-approved menus vs. your current food service costs.
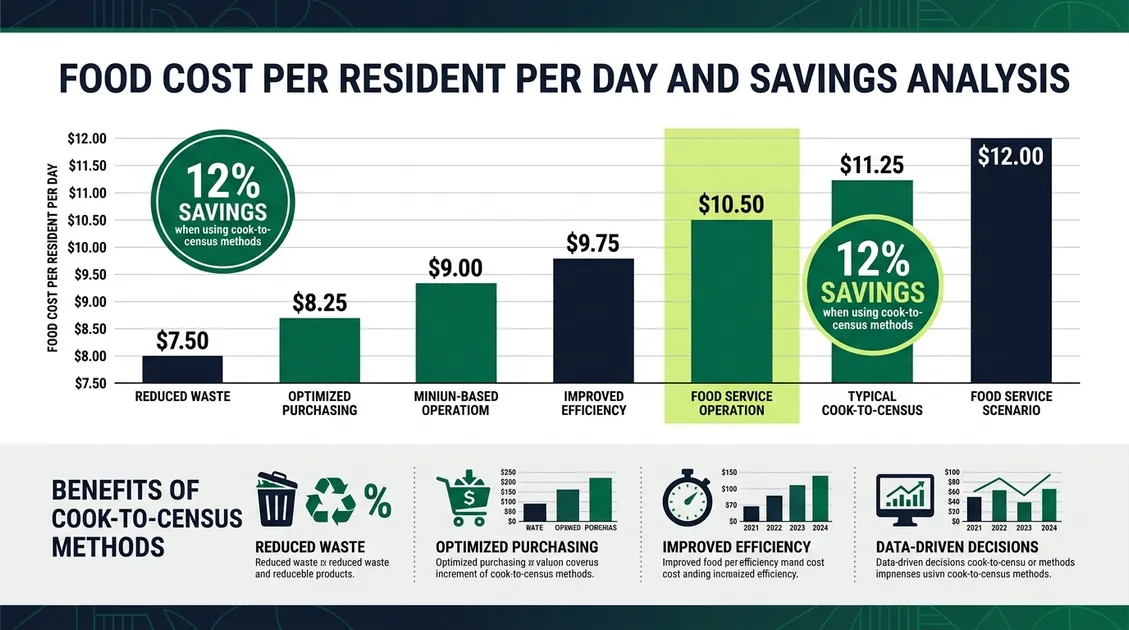
📊 Your Projected Annual Savings
How Does a 10-Week Rotating Menu Work in Assisted Living Settings?
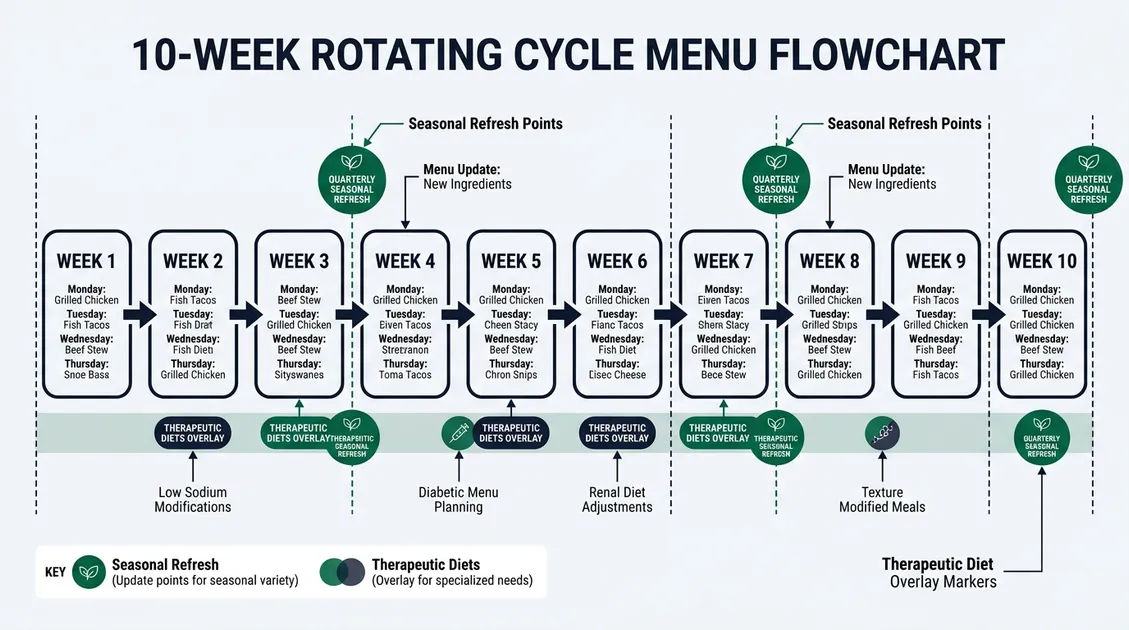
Assisted living residents consume an average of 1,800–2,100 calories daily with greater meal autonomy than skilled nursing populations, per the Journal of Nutrition in Gerontology and Geriatrics. A 10-week rotating cycle menu delivers 70 unique daily meal plans, breakfast. Lunch, dinner, and snacks before a single repeat, giving assisted living residents the dining variety they expect. PantryTec's 10-week rotation draws from a database of over 40,000 recipes across regular, therapeutic, and texture-modified categories. Each week's menu arrives as a PDF to your inbox with standardized recipes, portion-controlled ingredient lists, and production sheets. Seasonal updates refresh the rotation quarterly, including spring and summer produce or holiday menus for Thanksgiving and Christmas. The California HealthCare Foundation's home care research confirms that supportive housing with properly managed on-site services can reduce transfers to nursing homes and improve quality of life for elderly residents.

Adapting Cycle Length to Resident Expectations
Cycle menu length matters for resident satisfaction. A 4-week cycle repeats meals every 28 days, noticeable to long-term residents. PantryTec's 10-week rotation pushes that to 70 days.
Three menu styles give your kitchen additional flexibility: Homemade Focus for scratch-cooking kitchens. Premade Focus for facilities relying on convenience products, and Weekend Hybrid for operations that cook fresh on weekdays. You switch between styles anytime without extra fees.

Balancing Dining Choice With Nutritional Standards
Blake Oldham, PantryTec's Co-Founder, notes that assisted living operators often worry a dietitian-approved menu will feel institutional or bland, yet facilities using structured 10-week rotations report fewer dining complaints than those using ad hoc daily planning, based on our experience across 50+ food service operations. Each menu day hits DRI benchmarks for 28+ micronutrients including potassium, phosphorus, and iron while offering selective choices at lunch and dinner. A safety-net alternative menu ships every week for residents who decline the primary entrée. We cover this in detail in our cycle menus by facility type explained guide.
What Therapeutic Diet Options Are Available for Assisted Living Residents?
About 45% of assisted living residents manage at least one chronic condition requiring dietary change, according to the CDC's 2022 Long-Term Care Provider Survey, with diabetes at 29% and heart disease at 34% representing the most common triggers. PantryTec's therapeutic diet menus cover 8+ modified diet types including diabetic/consistent carb, renal, cardiac/low sodium, and IDDSI texture levels 4 through 6. Each therapeutic track layers directly onto your base cycle menu so kitchen staff execute one streamlined production plan not separate meal prep lines. A Registered Dietitian Nutritionist cross-references every therapeutic change against the base menu's nutrient analysis. Potassium-restricted renal menus hold intake below 2,000 mg/day. Cardiac menus limit sodium to 1,500–2,000 mg/day. Diabetic menus use PantryTec's Steady Carb strategy with standardized portions to prevent accidental carb loading at dinner.
Managing Diabetes, Heart Disease, and Renal Diets
Diabetic menus align with chrononutrition research, front-loading calories at the midday meal. Renal diet extensions track potassium, phosphorus, and fluid intake per meal. Cardiac/low-sodium menus stay under the USDA Dietary Guidelines for Americans threshold of 2,300 mg/day. The California HealthCare Foundation's home care report found that between 50 and 64 percent of RCFE residents needing help with mobility reported needing more help than they received, a finding that underscores how dietary management fills care gaps that physical staffing alone does not address.

Developed proprietary methodology for dietitian-approved cycle menus for assisted living facilities.
Texture Modifications and IDDSI Compliance
Therapeutic diet menus for senior care include IDDSI Level 4 (pureed), Level 5 (minced and moist), and Level 6 (soft and bite-sized) options. Dysphagia affects an estimated 15% of assisted living residents, creating aspiration risk when food textures don't match a speech-language pathologist's diet order. PantryTec's texture-modified menus maintain nutritional adequacy calorie and protein targets remain consistent regardless of IDDSI level.
Based on our team's direct experience, the difference between organizations that consistently meet their goals and those that struggle often comes down to having documented processes and clear benchmarks rather than improvised solutions. This practical insight drives PantryTec's approach. See dietary management guide for ALF administrators for a deeper breakdown.
Ready to Simplify Your Menu Compliance?
Get dietitian-approved cycle menus starting at $15/mo replace $750–$1,500/mo external dietitian costs. Covers 8+ therapeutic diets & 40,000+ recipes.
Ready to Get Started with PantryTec?
Contact PantryTec today to learn how we can help.
- Home
- Cycle Menus by Facility Type A Dietitian-Approved Senior Care Guide
- Dietitian Approved Menus for Assisted Living
