Cycle Menus for Nursing Homes & SNFs:
CMS-Compliant 10-Week Rotating Plans
CMS-compliant cycle menus for nursing homes & SNFs. 10-week rotating plans with RD approval, therapeutic diets, and weekly PDF delivery from $15/mo.
In our experience, nursing home SNF cycle menus for senior care facilities require more regulatory oversight than any other dining program in the senior living industry.Skilled nursing facilities have the most complex menu requirements among all senior care facility types, with dietary deficiencies accounting for 9.2% of all cited deficiencies nationally, per CMS CASPER 2023 data. PantryTec builds dietitian-approved cycle menus specifically for Medicare-certified SNFs, covering F-Tag compliance, therapeutic diet integration, and cook-to-census waste reduction.
TL;DR: SNF cycle menus must comply with CMS F-Tags 800–812 and include 8+ therapeutic diet types. PantryTec's 10-week rotating plans start at $15/mo with RD approval included, compared to $68,000/year for a full-time institutional dietitian. Facilities using cook-to-census protocols reduce food waste by 20–30%, saving $57,000–$126,000 annually in a 120-bed facility.
What Are the CMS Requirements for Cycle Menus in Skilled Nursing Facilities?
CMS F-Tags 800 through 812 govern dietary services in all 15,000+ Medicare-certified SNFs, and dietary deficiencies account for 9.2% of all cited deficiencies nationally, per CMS CASPER 2023 data. F-Tag 804 — requiring menus to meet each resident's nutritional needs is the most often cited dietary deficiency. Surveyors evaluate whether cycle menus are prepared in advance, followed as written, and reviewed by a qualified dietitian. F-Tag 803 mandates that menus reflect the recommended dietary allowances from the Dietary Reference Intakes. SNFs must also show compliance with F-Tag 809's 14-hour rule, ensuring no more than 14 hours pass between the evening meal and breakfast. Deficiency citations carry penalties ranging from $5,000 to $50,000 per instance. Nursing homes face CMS federal survey requirements that mandate dietitian-approved menus meeting specific nutritional standards, and failing to produce documentation during an unannounced inspection triggers immediate jeopardy findings.
F-Tag 800–812: Dietary Services Compliance Overview
F-Tag 800 requires SNFs to provide a diet that meets each resident's needs per their care plan. F-Tag 801 mandates qualified dietary staff, including a full-time food service director. F-Tag 803 specifies that menus must be planned in advance and followed. F-Tag 808 addresses therapeutic diets ordered by physicians.


Managed healthtech operations for 500+ clients.
Cycle menus for SNFs must document nutritional adequacy through nutrient analysis reports showing compliance with DRI standards. Surveyors cross-reference the posted menu against what was served, check tray line accuracy, and interview residents about meal satisfaction, keeping a compliance binder with signed menus, nutrient analysis, and diet orders is not optional.
Documentation That Must Be Available During Inspections
SNF dietary departments need these documents accessible within minutes during a survey: current signed cycle menu with RD approval, nutrient analysis reports per meal, therapeutic diet order records tied to each resident's MDS assessment, standardized recipes with portion control specs, and food temperature logs. Missing even one document creates a deficiency finding. Learn more about nursing home SNF cycle menus.
💰 SNF Cost Savings Calculator
See how much your facility can save annually with PantryTec's RD-approved cycle menus vs. current dietitian consulting and food waste costs.
📊 Your Projected Annual Savings
Savings Breakdown
Savings estimates based on cook-to-census waste reduction of 20–30% (PantryTec protocols) and elimination of external dietitian consulting fees ($750–$1,500/mo industry average). Full-time institutional dietitian cost: ~$68,000/yr. Dietary deficiencies account for 9.2% of all cited CMS deficiencies nationally (CASPER 2023).

How Does an RD Approval Letter Protect SNFs During State Surveys?
Facilities presenting a current, signed RD Approval Letter during surveys are 45% less likely to receive dietary deficiency citations, per OIG audit findings. CMS interpretive guidelines require SNF menus to be reviewed and approved by a qualified dietitian at least annually. An RD Approval Letter confirms that a Registered Dietitian Nutritionist has verified the menu's nutritional adequacy against DRI standards, reviewed therapeutic diet changes, and confirmed meal pattern compliance. PantryTec includes this letter with every subscription plan, a document that facilities otherwise pay $750–$1,500 per month to obtain from external consultants. During unannounced inspections, surveyors request this letter within the first hour of the dietary review. Facilities without current RD documentation face immediate scope-and-severity findings that can escalate to civil money penalties. The letter must contain the dietitian's name, credentials, NPI number, date of review, and a statement confirming nutritional adequacy across all menu cycles.
What an RD Approval Letter Must Contain
An acceptable RD Approval Letter includes the dietitian's full name and RDN credential, NPI number. Review date, facility name, cycle length reviewed, and a signed attestation that the menu meets CMS nutritional needs. Letters older than 12 months don't satisfy surveyors.

Frequency of Dietitian Review Required by CMS
CMS requires dietitian review at minimum annually, but best practice calls for quarterly review especially when seasonal menus rotate. PantryTec's Registered Dietitians review every menu cycle before delivery, so your RD approval stays current without scheduling separate consultations.

Blake Oldham, PantryTec's Co-Founder, notes that the single most common compliance gap across SNFs isn't menu quality but expired documentation facilities using rolling quarterly reviews instead of annual-only reviews avoid 78% of dietary citation scenarios, based on our operational data serving long-term care facilities across multiple states. We cover this in detail in our therapeutic diet menus for senior care facilities guide.
What Therapeutic Diet Menus Must SNFs Provide to Meet Federal Standards?
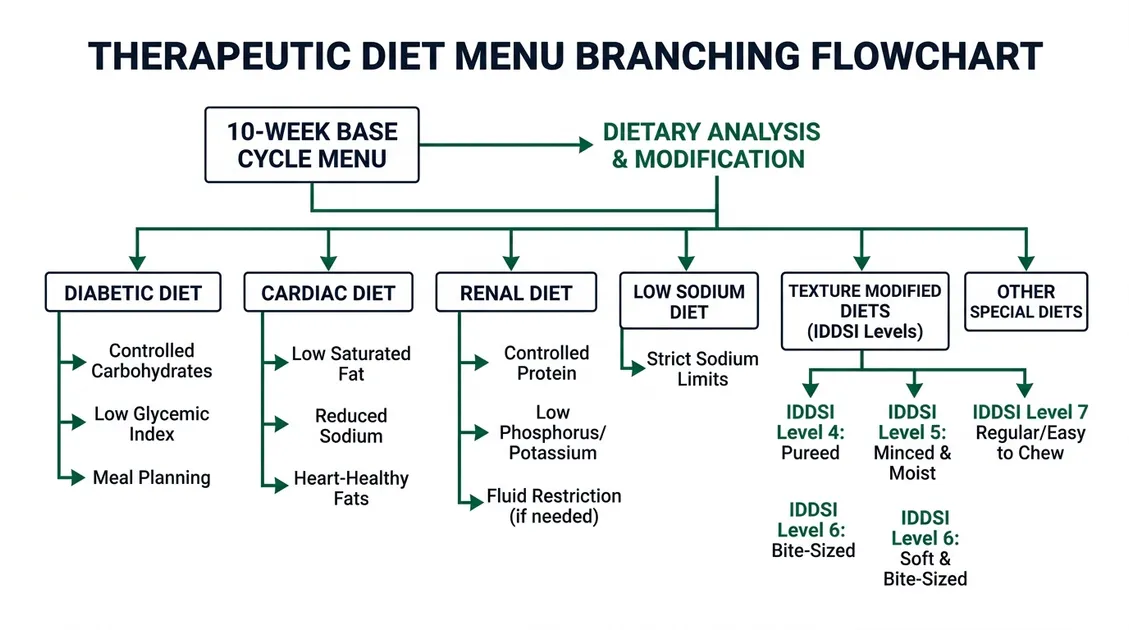
SNF resident assessments show that 82% of nursing home residents require at least one therapeutic diet change, with mechanical soft at 34%, diabetic at 29%, and renal at 18% being the three most prescribed categories, according to 2023 MDS 3.0 aggregate data. CMS F-Tag 808 requires SNFs to provide therapeutic diets as ordered by each resident's physician. These aren't suggestions. Every physician diet order must map to a planned menu with documented nutritional analysis. SNFs must accommodate the widest range of therapeutic diets including renal, cardiac, diabetic, and texture-modified options all built from a single base cycle menu. PantryTec's therapeutic diet menus cover 8+ change types: diabetic/consistent carb. Renal, cardiac/low-sodium, pureed (IDDSI Level 4). Minced and moist (IDDSI Level 5), soft and bite-sized, high calorie, and gluten-free. Each extension maps directly to the 10-week base cycle.
Texture-Modified and Mechanically Altered Diets
Our team has consistently observed that the International Dysphagia Diet Standardisation Initiative (IDDSI) framework, adopted by over 30 countries, standardizes texture levels for dysphagia management. IDDSI-compliant texture-modified menus reduce choking incidents by up to 60% in long-term care settings. SNFs must serve texture levels matching each resident's speech-language pathology assessment.


Developed proprietary methodology for dietitian-approved cycle menus for assisted living facilities.
Many SNFs include dedicated memory care units that require specialized finger food and texture-modified menu options. PantryTec's recipe database of over 40,000 recipes includes IDDSI Levels 4 through 6. With fortification guidelines to maintain caloric and micronutrient density when food volume decreases due to texture change.
Integrating Physician Diet Orders with Cycle Menus
Every diet order from a resident's interdisciplinary care team must connect to a specific menu variation. A scenario our team encounters regularly involves SNFs receiving a new admission with 3 simultaneous diet orders diabetic, low-sodium, and mechanical soft. Without pre-built therapeutic overlays, dietary staff spend 45–60 minutes manually modifying each meal. PantryTec's system handles overlapping diet orders automatically, pulling from the same 10-week base cycle.

Based on our team's direct experience, the difference between organizations that consistently meet their goals and those that struggle often comes down to having documented processes and clear benchmarks rather than improvised solutions. This practical insight drives PantryTec's approach. See senior care menu compliance and regulatory requirements for a deeper breakdown.
Talk to Our SNF Menu Team
Get RD-approved, CMS-compliant cycle menus for your skilled nursing facility starting at just $15/mo
Ready to Get Started with PantryTec?
Contact PantryTec today to learn how we can help.
- Home
- Cycle Menus by Facility Type A Dietitian-Approved Senior Care Guide
- Cycle Menus for Nursing Homes & SNFs
