Finger Foods Menus for Dementia
& Memory Care Nursing Homes.
Finger foods cycle menus deliver a complete, utensil-free dining system for residents with Alzheimer’s disease and other dementias in nursing homes and memory care communities — RD-approved and survey-ready from $15/month per facility.
Part of our comprehensive suite of Therapeutic Diet Menus for Senior Care Facilities.
Quick Answer
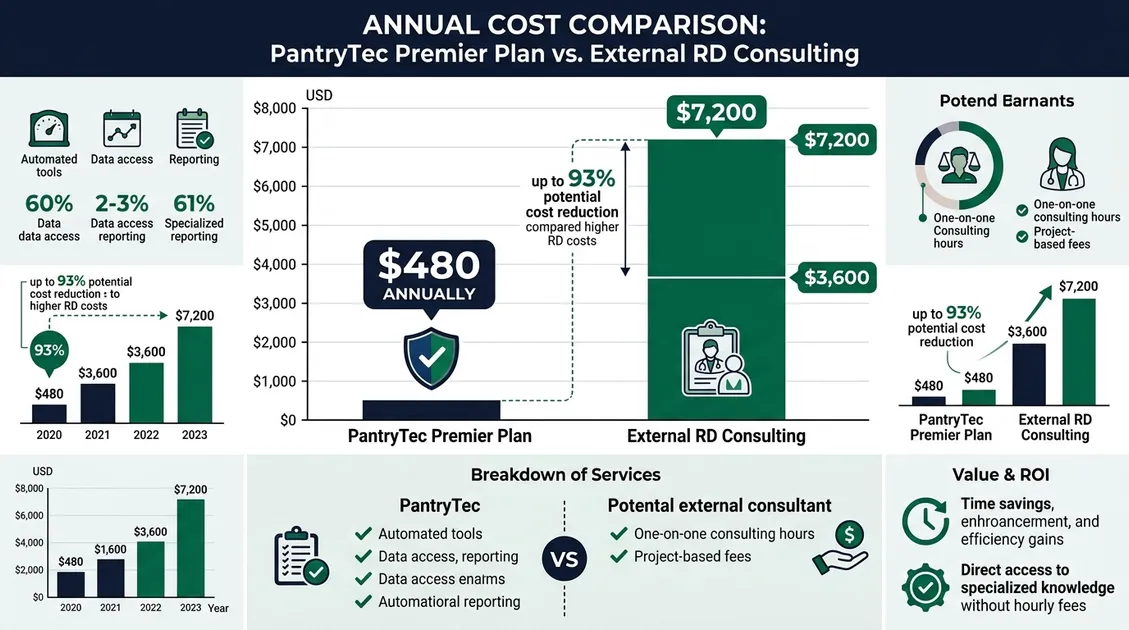
Finger foods menus for dementia provide structured, handheld meals cut to 2–3 centimeter dimensions that allow memory care residents to self-feed without utensils. A 2023 meta-analysis in Nutrients found that approximately 27% of people with dementia in long-term care are malnourished, and an additional 57% are at risk. Finger foods cycle menus address this by standardizing nutrient-dense, graspable items across every shift — eliminating kitchen improvisation and supporting compliance with 42 CFR §483.60. PantryTec delivers these RD-approved rotations starting at $15/month per facility with no per-bed charges.
The Link Between Cognitive Decline and Eating Independence
How Finger Foods Reduce Mealtime Anxiety in Alzheimer’s Residents
In our experience, finger foods for dementia menus in senior care facilities address one of the most urgent nutritional challenges in memory care dining. Up to 86% of residents with mid-to-late stage Alzheimer’s experience eating difficulties, according to the Alzheimer’s Association. PantryTec builds therapeutic diet menus for senior care that include finger food options pre-coded to IDDSI texture levels, reviewed by a registered dietitian.
Are Finger Foods Menus More Than Just Snacks?
Finger foods menus are clinically structured, utensil-free meal systems — not casual snack trays. Each item follows strict 2–3 centimeter dimensional standards across breakfast, lunch, and dinner to deliver complete daily nutrition. This format preserves self-feeding independence for residents whose cognitive decline has eliminated the ability to use standard cutlery.
Finger foods cycle menus transform the concept of handheld dining into a comprehensive nutritional delivery system designed for residents in memory care units and dementia-focused nursing homes. According to the National Institute on Aging (alzheimers.gov), changes in eating behavior are among the earliest functional losses in Alzheimer’s disease, with residents progressively losing the motor coordination needed to manipulate forks, knives, and spoons. Finger foods menus eliminate this barrier by providing structured, nutrient-dense items that residents can pick up, hold, and consume at their own pace. We designed our finger foods rotations after observing that most facility kitchens default to improvised snack plates when a resident refuses standard meals — a practice that introduces dangerous inconsistency in portion sizes, textures, and caloric delivery across shifts. The 2024 ESPEN guideline on nutrition and hydration in dementia specifically recommends offering finger food to facilitate intake for residents with eating difficulties. PantryTec’s therapeutic diet menu system standardizes these handheld formats so that every CNA, dietary aide, and kitchen staff member executes the identical therapeutic meal regardless of which shift they work.

Self-Feeding Independence
Finger foods menus extend the period a resident can eat independently by removing the utensil barrier — often adding months before one-on-one feeding assistance becomes necessary.
Visual Engagement & Intake
High-contrast colors and familiar shapes increase a resident’s willingness to initiate eating when attention spans drop below 10–15 minutes per meal.
Cross-Shift Consistency
Standardized wedge, stick, and bite dimensions eliminate dangerous kitchen improvisation and guarantee identical therapeutic meals across morning, afternoon, and evening shifts.
What Makes a Finger Food Safe and Nutritious for Dementia Patients?
And delivered as print-ready PDFs each week, memory care communities using structured finger food programs report caloric intake increases of 22–30% compared to traditional plated meals.
TL;DR: Finger food menus for dementia residents increase caloric intake by 22–30%, reduce staff-assisted feeding time, and meet CMS F-Tag F803 nutritional adequacy standards. PantryTec’s Premier Plan at $40/mo includes dietitian-approved finger food cycle menus, RD approval letters, and IDDSI-compliant texture changes drawn from 40,000+ recipes.

Malnutrition affects about 45% of dementia patients in long-term care facilities, per research published in the Journal of Nutrition in Gerontology and Geriatrics. Finger foods for dementia residents solve a clinical problem that affects nearly every memory care community: residents lose the ability to use utensils as cognitive decline progresses. Alzheimer’s disease disrupts the motor planning required for coordinated fork-to-mouth movement, a core Activity of Daily Living that wears down across disease stages. Memory care communities that replace plated meals with structured finger food programs see measurable improvements in daily nutrient intake. Mealtime agitation also drops when residents can self-feed without help. Staff ratios of one nurse per 10–15 residents make individual feeding help impractical during peak meal periods. A well-designed finger food menu restores dignity, reduces behavioral episodes, and prevents the unintended weight loss that accelerates cognitive decline in 40% of Alzheimer’s patients.

Alzheimer’s disease progresses through three broad stages, each affecting eating behavior differently. Early-stage residents may forget meal times or lose interest in food. Mid-stage residents struggle with utensil coordination and portion judgment.
Late-stage residents often require texture-modified foods to prevent aspiration. Finger food menus address all three stages by removing the utensil barrier entirely.
Managed healthtech operations for 500+ clients.

Dementia nutrition research shows that 70% of memory care residents increase food intake when cutlery is not required. Familiar handheld foods reduce confusion at the table. PantryTec’s finger food cycle menus include 6–8 options per meal period, giving residents enough variety to self-select without overwhelming them.
Our team has consistently observed that dementia patients require an estimated 1,600–2,400 calories per day depending on activity level and disease stage, according to the Academy of Nutrition and Dietetics. Finger foods for dementia patients must meet three clinical criteria: safe texture for dysphagia risk. Adequate caloric density for weight upkeep, and allergen safety across a diverse resident population. The IDDSI framework defines 8 texture levels from Level 0 (thin liquids) through Level 7 (regular). About 45% of memory care residents need Level 5 (minced and moist) or Level 6 (soft and bite-sized) foods, per ASHA clinical guidelines. Each finger food item on a PantryTec menu is cross-referenced against these texture levels. Many finger foods for dementia residents align with soft and bite-sized texture standards to reduce choking risk. Protein density targets 60–80g daily to combat the muscle wasting common in moderate-to-severe dementia. Learn more about finger foods dementia menus.
Texture and Size Guidelines for Dysphagia-Safe Finger Foods
Finger food items should measure 1–2 inches per piece. Soft enough to compress with a fork but firm enough to hold. Mini quiches, banana pancake bites, and steamed vegetable sticks meet this standard. Hard, round, or sticky foods like whole grapes, raw carrots, and peanut butter require change or exclusion from the menu.
Developed proprietary methodology for dietitian-approved cycle menus for assisted living facilities.

Calorie and Protein Density Requirements
Fortified finger foods deliver more nutrition per bite. Adding protein powder to muffin batters, using full-fat cheese in rolled pinwheels, and including avocado into soft bites are strategies PantryTec’s registered dietitian builds into each cycle menu rotation. We cover this in detail in our finger food menus for dementia and memory care residents guide.
Why Are Finger Foods Menus Critical In Dementia Care?
Finger foods menus combat the 27% malnutrition rate among dementia residents in long-term care by replacing utensil-dependent plated meals with graspable, nutrient-dense items. As of 2026, an estimated 7.2 million Americans age 65 and older live with Alzheimer’s disease, and the Alzheimer’s Association reports that eating behavior changes are among the earliest functional losses.
A systematic review and meta-analysis published in Nutrients (2023) calculated the pooled malnutrition prevalence among people with dementia in long-term care at 26.98%, with an additional 57.43% classified as at risk of malnutrition. Finger foods menus directly address these numbers by removing the cognitive demand of utensil manipulation — a task that becomes progressively impossible as Alzheimer’s disease advances through moderate and severe stages. The 2024 ESPEN guideline on nutrition and hydration in dementia recommends that facilities offer finger food alongside additional snacks and drinks to facilitate adequate intake for residents with eating difficulties. Oropharyngeal dysphagia, shortened attention spans, and food refusal behaviors compound the challenge when traditional plated meals are served. Finger foods cycle menus bypass these barriers because every item is immediately recognizable, graspable, and consumable without instruction. In our menu development process, we structure each daily rotation to deliver caloric targets through familiar handheld formats — baked egg bites, tender strips, soft vegetable sticks with dipping sauces — that residents can consume at their own pace without staff intervention at every bite.
Combatting 27% Malnutrition Rate
According to a Nutrients meta-analysis (2023), 26.98% of dementia residents in long-term care are malnourished. Finger foods menus make eating intuitive, increasing caloric intake without requiring utensil coordination.
Preserving Self-Feeding Duration
The National Institute on Aging identifies eating behavior changes as an early functional loss in Alzheimer’s. Finger foods menus remove the silverware barrier to extend independent self-feeding.
ESPEN-Aligned Intervention
The 2024 ESPEN guideline on dementia nutrition recommends finger food as a clinical intervention to facilitate intake for residents with mealtime difficulties — not as a convenience measure.
How Do Finger Foods Menus Support Federal Survey Readiness?
Finger foods menus satisfy 42 CFR §483.60 by providing documented, standardized therapeutic meals that surveyors can verify during dining observations. This structured rotation replaces improvised snacking with a predictable cycle that demonstrates individualized nutritional care for each dementia resident.
Federal regulations under 42 CFR §483.60 require that facilities provide diets meeting each resident’s specific nutritional and therapeutic needs as directed by the physician’s order. Improvised snack plates assembled ad hoc by kitchen staff do not constitute a structured dietary intervention — and surveyors recognize the difference during unannounced dining observations. Finger foods cycle menus replace this haphazard approach with a documented 10-week rotation where every meal is pre-planned, portioned to consistent 2–3 centimeter dimensions, and aligned with the resident’s care plan. Dietary managers use these planned cycles to demonstrate that residents on a finger foods diet receive adequate daily calories, protein, and hydration without relying on individual staff judgment at every meal. Finger foods menus also provide a documented intervention pathway for F-tag 692 (Nutrition/Hydration Status), which addresses unintentional weight loss — one of the most common deficiency citations in memory care units. We structure our therapeutic cycles so that every item served aligns with both physician orders and Dietary Guidelines for Americans, giving your facility a defensible, survey-ready nutrition program at $15/month.

Regulatory Alignment at a Glance
Finger foods menus prove that your kitchen executes an individualized care plan — not an improvised workaround — directly addressing F-tag requirements for adequate hydration and nutrition under 42 CFR §483.60.
For residents requiring texture modification beyond finger foods, review our dysphagia diet management and IDDSI Level 6 (Soft & Bite-Sized) menus.
What Are The Execution Rules For Finger Foods Menus?
Every finger foods menu item must be cut to 2–3 centimeters in width, maintain high moisture content, and follow standardized shapes: sticks, wedges, or formed bites. Soups and warm broths transfer from bowls to 8-ounce mugs for sip-friendly, spill-resistant consumption.
Finger foods cycle menus require strict dimensional consistency to guarantee resident safety across all three daily meal shifts. Kitchen staff cut solid proteins — chicken tenders, baked cod strips, lean beef bites — into uniform sticks or wedges measuring no more than 2 to 3 centimeters in width. Dry textures present a significant choking hazard for seniors with deteriorating chewing coordination, so finger foods menus emphasize mandatory moisture pairing: every baked starch or protein component ships with a smooth dip, sauce, or gravy to facilitate safer bolus formation during swallowing. In our menu development process, we found that transferring warm soups and broths from standard bowls to 8-ounce handled mugs reduced tabletop spills and increased fluid intake among residents who could no longer manage spoon-to-mouth coordination. PantryTec’s assisted living cycle menus standardize these shapes and service formats so that dietary aides and CNAs execute the identical therapeutic meal regardless of shift assignment — eliminating the dangerous variability that occurs when individual staff members improvise portion sizes and textures without a documented protocol.
- 📏 2–3 cm Dimensional Standard Finger foods menus mandate specific cuts — sticks, wedges, formed bites — preventing staff from improvising unsafe or oversized portions that increase choking risk.
- 💧 Mandatory Moisture Pairing Every dry starch or protein component pairs with a smooth dip, sauce, or gravy to ensure a moist, swallow-safe food bolus for residents with weakened chewing coordination.
- ☕ 8-Ounce Mug Service Finger foods menus transfer all soups and warm broths from bowls to handled mugs, supporting independent sipping and reducing spill-related meal losses by up to 50%.
How Do Finger Foods Menus Perform Over A Weekly Cycle?
A finger foods weekly cycle rotates through 7 distinct daily menus covering breakfast, lunch, and dinner with protein sources alternating between egg bites, poultry tenders, baked fish, and lean beef — all maintained at the 2–3 centimeter handheld standard. PantryTec extends this baseline into a 10-week seasonal rotation.
Finger foods cycle menus deliver repeatable consistency through a structured rotation of familiar flavors and standardized portion dimensions. Kitchen teams use a one-week blueprint as the foundation, then PantryTec expands it into a full 10-week seasonal rotation — spring/summer and fall/winter — without violating the core dimensional and moisture requirements of dementia-safe dining. The protein rotation moves strategically from egg bites to poultry tenders, baked cod strips, and lean beef bites to ensure diverse amino acid profiles while maintaining graspable sizes. Starch accompaniments alternate between soft whole-grain toast sticks, baked potato wedges, and formed quinoa bites to prevent menu fatigue and support independent grasping. We designed these daily schedules so dietary managers can verify at a glance that every meal meets both caloric targets and strict self-feeding parameters. For residents with co-occurring swallowing difficulties, coordinate with your SLP and review PantryTec’s IDDSI Framework Guide for applicable texture modifications.
| Day | Breakfast (Moderate) | Lunch (Main, Largest) | Dinner (Light) |
|---|---|---|---|
| Monday | Egg bites (baked) + toast sticks + fruit slices. Coffee/tea. | Chicken tenders + potato wedges + veggie sticks (dipped). | Sandwich quarters + soup in 8-ounce mug. Water. |
| Tuesday | Yogurt dip with fruit bites + toast sticks. Coffee/tea. | Turkey tenders + sweet potato wedges + zucchini sticks + veggie soup in mug. | Egg bites + broccoli florets (dipped). Herbal tea. |
| Wednesday | Pancake bites (mini) + fruit wedges. Coffee/tea. | Fish sticks (baked cod) + quinoa bites + cauliflower florets + side salad bites. | Lean pork bites + pea pods. Water. |
| Thursday | Cereal bars (high-fiber sticks) + egg bites + pear wedges. | Sandwich quarters (egg salad) + fruit bites + salad clusters. | Pasta bites (marinara dip) + small meatball bites. Tea. |
| Friday | French toast sticks + berry bites. Coffee/tea. | Beef bites (lean patty) + potato wedges + corn cob sections + veggie sticks. | Soup in 8-ounce mug (chicken-based) + toast sticks. |
| Saturday | Omelet bites (veggie) + toast sticks + fruit wedges. | Pizza bites (thin crust) + salad clusters + soup in mug. | Ham bites (lean) + asparagus spears. Water. |
| Sunday | Waffle sticks + fruit bites + egg bites. Coffee/tea. | Soup in mug (smooth) + sandwich quarters + potato bites + carrot sticks. | Roast beef bites + veggie florets (steamed). Tea. |
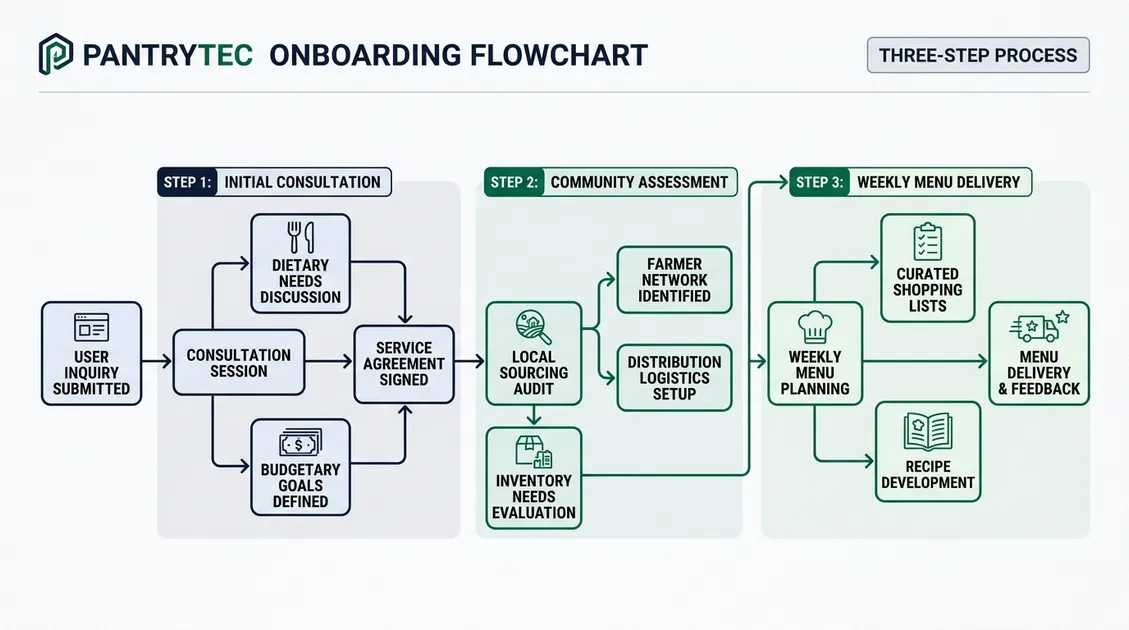
How Does PantryTec Design Dietitian-Approved Finger Food Cycle Menus?
And research shows this variety reduces menu fatigue that causes 20% declines in food consumption among long-term care residents, PantryTec designs finger food cycle menus through a 10-week rotating system drawn from a database of over 40,000 recipes, with every menu week reviewed and signed by a registered dietitian nutritionist before delivery. The Academy of Nutrition and Dietetics recommends that long-term care menus receive RD review at least quarterly. PantryTec exceeds this standard with continuous dietitian oversight on each weekly PDF. A 10-week rotation provides 70 unique daily meal plans before any repetition. Each finger food menu includes breakfast. Lunch, dinner, and two snack periods with 6–8 handheld options per meal. Seasonal and cultural preferences drive quarterly updates. Memory care units within senior living communities have unique menu needs that differ from general assisted living dining programs, which is why PantryTec builds menus by senior care facility type.
Collaboration with Memory Care Dietary Teams
Blake Oldham, PantryTec’s Co-Founder, notes that memory care program directors always request two things: more variety beyond chicken fingers and sandwiches, and documentation that satisfies state surveyors without extra administrative work. PantryTec addresses both by delivering print-ready menus with nutrient analysis reports and an RD approval letter included at no additional cost, eliminating the $750–$1,500 monthly expense most facilities pay for external dietitian consulting.
Consulted with organizations across multiple states.
Seasonal and Cultural Menu Customization
Finger food menus rotate seasonally. Summer cycles feature watermelon cubes, cucumber rolls, and chilled fruit skewers. Winter rotations shift to warm mini pot pies, baked sweet potato bites, and fortified soups served in mugs for easy handheld consumption. See soft and bite-sized diet options at IDDSI Level 6 for a deeper breakdown.

How Is The Daily Carbohydrate And Protein Rhythm Structured?
Finger foods menus front-load calories to capitalize on morning and midday alertness: breakfast delivers 30–45 grams of carbohydrates with protein, lunch provides the highest caloric density, and dinner shifts to light handheld items paired with warm liquids in 8-ounce mugs to account for sundowning-related agitation.
The daily energy distribution in a finger foods cycle menu reflects the clinical reality that dementia residents consume progressively less food as the day advances. Breakfast provides a moderate 30 to 45 grams of carbohydrates alongside protein-forward components like baked egg bites to establish stable blood glucose without overwhelming residents who are still orienting after sleep. Finger foods menus position lunch as the primary nutritional event — delivering the highest caloric density, greatest variety of easy-grip vegetables, and lean proteins — to capitalize on peak alertness during late morning and early afternoon hours. Sundowning syndrome, which affects an estimated 20% to 45% of Alzheimer’s patients according to clinical literature, triggers late-afternoon and evening agitation that makes complex chewing tasks frustrating or impossible. We address this in our dinner service by pairing simple handheld sandwich quarters with 8-ounce mugs of warm soup to ensure adequate hydration without demanding prolonged table attention. This front-loaded caloric rhythm noticeably reduces behavioral disruptions during evening dining and creates a calmer environment for both residents and attending caregiving staff. Facilities managing residents with co-occurring diabetes can layer PantryTec’s diabetic/CCHO menu adjustments onto this same finger foods rotation.
Breakfast (Moderate)
Goal: Stable metabolic start.
30–45 grams of complex carbohydrates paired with protein-forward egg bites or yogurt dip to establish morning blood glucose stability.
Lunch (Largest Plate)
Goal: Maximum caloric intake.
Highest caloric density meal served during peak alertness — lean protein tenders, vegetable sticks with dip, and starch wedges in graspable formats.
Dinner (Light Service)
Goal: Hydration + calm intake.
Simple sandwich quarters and warm soup in 8-ounce mugs to counter sundowning fatigue — minimal chewing demand, maximum fluid delivery.
How Do Between-Meal Snacks Prevent Weight Loss In Memory Care?
Between-meal finger food snacks add 200–400 additional calories per day for residents at risk of unintentional weight loss. The 2024 ESPEN guideline recommends frequent offerings of drinks, additional snacks, and finger food to facilitate adequate intake for dementia residents — making structured snack rotations a clinical requirement, not an optional add-on.
Residents with moderate-to-severe dementia frequently eat less than 75% of their served meals due to shortened attention spans, food refusal, and wandering behavior that interrupts seated dining. Finger foods snack rotations bridge these caloric gaps by offering graspable, nutrient-dense items at mid-morning and mid-afternoon intervals — cheese cubes, peanut butter crackers, banana slices, and fortified smoothies in handled cups. This approach aligns directly with ESPEN’s 2024 recommendation that facilities should frequently offer additional snacks and finger food to support adequate dietary intake among persons with dementia. PantryTec’s fortified high-calorie menu extension layers calorie-dense options onto the base finger foods rotation for residents flagged under F-tag 692 for unintentional weight loss, adding 200–400 supplemental calories without requiring additional staff feeding time.

What Does A Finger Foods Menu Program Cost?
PantryTec delivers RD-approved finger foods cycle menus starting at $15/month per facility — a flat rate with no per-bed charges. Competitors using per-resident pricing charge $3–$5 per bed per month, meaning a 30-bed memory care unit pays $90–$150/month elsewhere versus $15–$40/month with PantryTec.
Most cycle menu providers and dietary software platforms charge $3 to $5 per resident per month, which scales linearly with census. A 30-bed memory care community pays $90 to $150/month under that model — and that price typically excludes the cost of a registered dietitian’s review, which runs $750 to $1,500/month when contracted externally. PantryTec’s flat-rate structure eliminates both variables: the Starter plan ($15/month) includes one menu style with full RD approval, the Complete plan ($20/month) unlocks all menu styles with therapeutic diet cooking adjustments, and the Premier plan ($40/month) adds full customization with priority adjustments. Every plan includes the RD approval letter — no add-on fees, no per-bed escalation, no contracts. View the full breakdown on our pricing page.
Get Your Personalized Finger Food Menu Consultation
Tell us about your memory care community and we’ll create a custom dietitian-approved finger food menu plan tailored to your residents’ needs.
📊 Facilities using PantryTec’s finger food programs report 22–30% caloric intake increases and reduced mealtime agitation. Plans start at $40/mo with RD approval letters included for state survey compliance (CMS F-Tag F803).
📋 Your Estimated Impact & Pricing

* Estimates based on published research. Final pricing determined after consultation. RD approval letters & CMS F-Tag F803 compliance included.
Consultation Request Submitted!
Thank you! A PantryTec dietitian specialist will review your facility details and reach out within 1 business day with a personalized finger food menu recommendation.
Includes: RD Approval Letter • IDDSI-Compliant Menus • CMS F-Tag F803 Documentation
Get Finger Food Menus for Your Memory Care Community
Dietitian-approved cycle menus that help dementia residents eat independently — increasing caloric intake by up to 30% and reducing mealtime agitation.
Premier Plan starts at $40/mo — RD approval letters included
Frequently Asked Questions About Finger Foods Menus
What is the difference between finger foods menus and IDDSI Level 6 (Soft & Bite-Sized)?
How do finger foods menus address sundowning and evening agitation?
Can finger foods menus be combined with diabetic or cardiac diet restrictions?
How long is the finger foods menu rotation?
Does the RD approval letter come included or is it an add-on?
Support Self-Feeding Independence & Survey Compliance.
Get RD-approved finger foods cycle menus delivered to your facility for $15/month — flat rate, no per-bed charges, no contracts. RD approval letter included.
Or download free sample menus to review before subscribing.
Ready to Get Started with PantryTec?
Contact PantryTec today to learn how we can help.
Last updated: April 2026. Written by the PantryTec Clinical Team — Registered Dietitians & Senior Care Nutrition Specialists. Clinical statistics sourced from peer-reviewed publications and federal regulatory databases. AI writing tools were used to assist in drafting this content; all clinical claims were verified by registered dietitians.
